Background
Nevus sebaceus (sebaceous nevus), a circumscribed hamartomatous lesion predominantly composed of sebaceous glands, was first described by Jadassohn in 1895. It is a rare benign tumor in children that usually presents with warty patches of hair loss on the scalp (see the image below). Sebaceous nevi and verrucous epidermal nevi are closely related, and many authors regard them as variants.
Nevus sebaceus is a rare benign tumor in children that usually presents with warty patches of hair loss on the scalp.
The development of secondary malignant neoplasms within the nevus sebaceus is rare and occurs almost exclusively in adults. Possible signs of malignancy include ulceration or a new "bump" on the area; thus if any change is seen within the nevus sebaceus, patients should seek medical advice. Given the low risk of malignant transformation in children, clinical follow-up is considered to be a safe alternative to prophylactic surgical excision in pediatric patients.
If treatment is chosen, surgical excision would be the treatment of choice [1] ; however, the timing of surgery is controversial. [2] Factors to be considered include the size and location of the nevus, its cosmetic significance, and the risks and benefits of early excision (which usually requires general anesthesia) vs delayed excision (which usually requires only local anesthesia). Laser ablation has been employed for treatment as well. [3]
Pathophysiology
In nevus sebaceus, postzygotic somatic mutations may result in various clinical expressions of mosaicism. Mutations in pluripotential cells may give rise to hamartomas with multiple cell lines.
Etiology
Familial cases of sebaceous nevus have been reported. [4, 5, 6] Mutations in pluripotential cells during embryogenesis may generate varying lines of differentiation included in organoid nevi. Nevus sebaceus appears to respond to hormonal influences; the lesion can be raised at birth, become flattened in childhood, and become raised again during puberty.
Deletions of the patched gene have been identified in nevus sebaceus and may be responsible for the predisposition to the development of basal cell carcinoma (BCC) and other tumors in this lesion.
Epidemiology
In the United States, nevus sebaceus occurs with equal frequency in males and females of all races; it affects 0.3% of newborns. Worldwide, sebaceous nevi are sporadic and occur with equal frequency in males and females of all races.
Nevus sebaceus is usually noted as a solitary lesion at birth or in early childhood, whereas the characteristic features may not develop until puberty.
Prognosis
The medical importance of a solitary nevus sebaceus relates to the description of both benign change and, in some cases, malignant neoplastic change. Whereas earlier studies reported malignant transformation rates in the range of 10-15%, subsequent studies demonstrated that the rate is certainly less than 1% and that transformation nearly always occurs after puberty. In older reports, many lesions misdiagnosed as BCCs were in fact trichoblastomas (benign neoplasms that resemble BCC histologically).
The most common malignant neoplasm arising in this disorder is BCC, but the development of this or any other malignant neoplasm is uncommon. The most frequent benign tumors are trichoblastomas and syringocystadenoma papilliferum, occurring in fewer than 5% of patients with nevus sebaceus. [7]
Other benign and malignant tumors include apocrine cystadenoma, leiomyoma and sebaceous cell carcinoma. Rarely, malignant eccrine poromas, sebaceous carcinomas, and apocrine carcinomas have been reported to result in widespread metastases and death.
-
Nevus sebaceus in a 4-month-old baby manifesting as nodular plaque.
-
Brownish wartlike plaque in a 25-year-old patient.
-
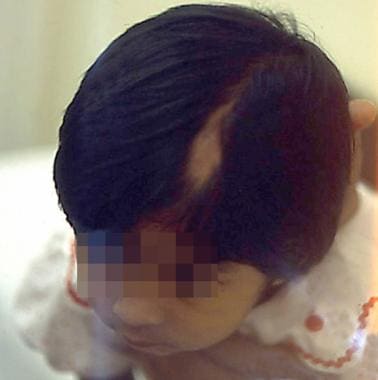
Nevus sebaceus manifesting as a bald patch in a child.
-
Nevus sebaceus manifesting as an orange-yellow plaque with a smooth or somewhat velvety surface in a 6-month-old baby.
-
Nevus sebaceus manifesting as a small plaque beside a scaly scalp in a 13-year-old boy.
-
Linear type of nevus sebaceus.
-
Mild papillomatosis of the epidermis with sebaceus gland lobules opening directly onto the epidermis.
-
Mild papillomatosis at high power.
-
Verrucous plaque in a 19-year-old woman.
-
Verrucous plaque in a 12-year-old-girl.