Background
Fractures of the hip are relatively common in adults and often lead to devastating consequences. Disability frequently results from persistent pain and limited physical mobility. Most hip fractures occur in elderly individuals as a result of minimal trauma, such as a fall from standing height. In young, healthy patients, these fractures usually result from high-velocity injuries, such as motor vehicle collisions or falls from significant heights. Despite comparable fracture locations, the differences in low- and high-velocity injuries in older versus younger patients outweigh their similarities. High-velocity injuries are more difficult to treat and are associated with more complications than minor trauma injuries.
Skeletal Anatomy
The hip joint is a large multiaxial ball-and-socket synovial joint, enclosed by a thick articular capsule. The hip joint is designed for stability and a wide range of movement. Next to the shoulder, it is the most moveable of all joints. During standing, the entire weight of the upper body is transmitted to the heads and necks of the femurs. The round head of the femur articulates with the cuplike acetabulum. The depth of the acetabulum is increased by the reinforcing fibrocartilaginous labrum, which "grasps" the femoral head, covering more than half of it. Articular cartilage covers the entire head of the femur, except for the pit (fovea) for the ligament of the femoral head.
The strong, loose fibrous capsule permits free movement of the hip joint, attaching proximally to the acetabulum and transverse acetabular ligament. The fibrous capsule attaches distally to the neck of the femur only anteriorly at the intertrochanteric line and root of the greater trochanter. Posteriorly, the fibrous capsule crosses to the neck proximal to the intertrochanteric crest without attaching to it. The fibrous capsule thickens to form 3 ligaments of the hip joint: the Y-shaped iliofemoral ligament (of Bigelow), the pubofemoral ligament, and the ischiofemoral ligament.
The hip joint is further supported by the femur and the muscles that cross the joint; this bone and these muscles are the largest and most powerful in the human body. (The anatomy of the femur is shown below.)
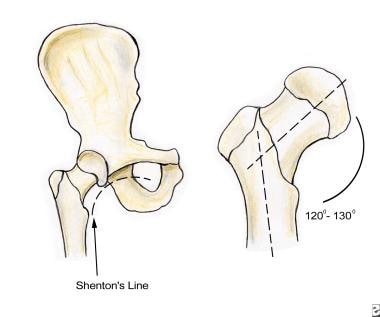
The length, angle, and narrow circumference of the femoral neck permit substantial range of motion at the hip but also subject the femoral neck to incredible shearing forces. A fracture results when these forces exceed the strength of the bone. The intertrochanteric line is an oblique line that connects the greater and lesser trochanters, dividing the femoral neck from the shaft. Hip fractures involve fracture of any aspect of the proximal femur, from the head to the first 4-5 cm of the subtrochanteric area.
Vascular Supply
The vascular supply to the proximal femur is tenuous and provided largely by 2 sources. Branches of the medial and lateral circumflex femoral arteries, usually branches of the deep femoral artery, ascend on the posterior aspect of the femoral neck in the retinacula (reflections of the capsule along the neck of the femur toward the head). The branches of the medial and lateral circumflex arteries perforate the bone just distal to the head of the femur, where they anastomose with branches from the foveal artery and with medullary branches located within the shaft of the femur.
The ligament of the head of the femur usually contains the artery of the ligament of the head of the femur (foveal artery), a branch of the obturator artery. The foveal artery enters the head of the femur only when the center of the ossification has extended to the pit (fovea) for the ligament of the head, around age 11-13 years. This anastomosis persists even in advanced age but is never established in 20% of the population.
Femoral neck fractures often disrupt the blood supply to the head of the femur. The medial circumflex artery supplies most of the blood to the head and neck of the femur and is often torn in femoral neck fractures. In some cases, the blood supplied by the foveal artery may be the only blood received by the proximal fragment of the femoral head. If the blood vessels are ruptured, the fragment of bone may receive no blood and undergo avascular necrosis (AVN).
Classifying Fractures
Hip fractures can be classified based on their relation to the hip capsule (intracapsular and extracapsular), geographic location (head, neck, trochanteric, intertrochanteric, and subtrochanteric), and degree of displacement. Higher-grade displacement implies worse prognosis. Fractures of the femoral head and neck are intracapsular, whereas those of the trochanteric, intertrochanteric, and subtrochanteric regions are extracapsular. The treatment, as well as the prognosis for successful union and restoration of normal function, varies considerably with fracture type.
Intracapsular hip fractures, like all other intracapsular fractures, frequently have complicated healing. The thick capsule that surrounds these fractures separates them from adjacent soft tissue and capillaries, leading to impaired callous formation. Thus, nonunion and AVN are added complications of these fractures.
Femoral head fractures
Isolated femoral head fractures are rare and are usually associated with hip dislocations. Superior femoral head fractures are normally associated with anterior dislocations, while inferior femoral head fractures are associated with posterior dislocations. They are usually best appreciated on postreduction radiographs for hip dislocations. Fractures of the femoral head are more common in younger patients as a result of major trauma, which is more likely to cause femoral neck fractures in older patients.
A type 1 fracture is a single fragment fracture, and type 2 is a comminuted fracture (see image below).
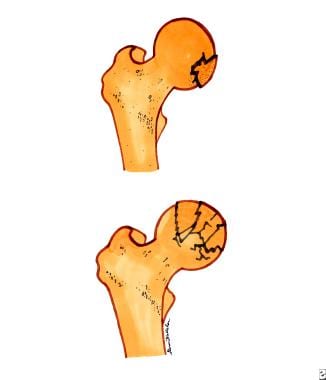 Femoral head fractures. Top diagram is a single-fragment femoral head fracture. Bottom diagram is a comminuted femoral head fracture.
Femoral head fractures. Top diagram is a single-fragment femoral head fracture. Bottom diagram is a comminuted femoral head fracture.
Femoral neck fractures
Femoral neck fracutures are rare in younger patients and more commonly seen in older adults, most often secondary to osteoporosis or osteomalacia. These fractures usually result from minor trauma, with falls accounting for 90%, or torsion. From proximal to distal, femoral neck fractures can be further delineated as subcapital, transcervical, and basicervical, all of which are intracapsular and are associated with potential disruption of the vascular supply. The incidence of avascular necrosis (AVN) is up to 15% in nondisplaced fractures and increases to nearly 90% with untreated, completely displaced fractures.
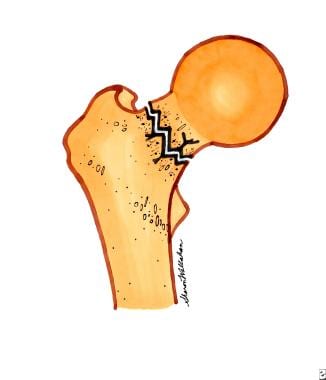
Type 1 is a stress fracture or incomplete fracture, and type 2 is an mpacted fracture (see image below).
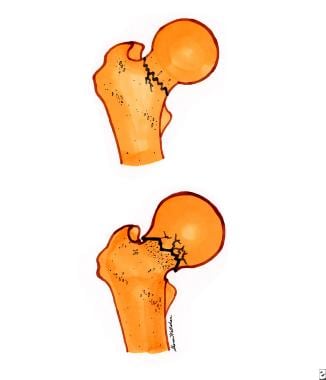 Femoral neck fractures. Top diagram is a nondisplaced, or incomplete, femoral neck fracture. Bottom diagram is an impacted femoral neck fracture.
Femoral neck fractures. Top diagram is a nondisplaced, or incomplete, femoral neck fracture. Bottom diagram is an impacted femoral neck fracture.
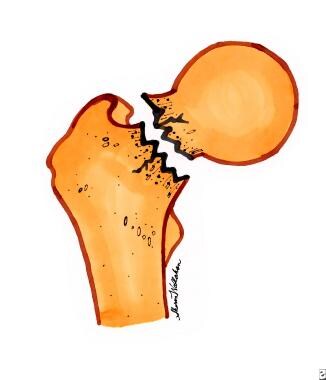
Type 3 is a partially displaced fracture (see image below).
Type 4 is a completely displaced or comminuted fracture (see image below).
Trochanteric fractures
Greater trochanteric fractures usually result from avulsion injuries at the insertion of the gluteus medius. Lesser trochanteric fractures may be caused by avulsion injuries of the iliopsoas secondary to forceful contraction. These are most common in children and young athletes (eg, dancers, gymnasts).
Type 1 is a nondisplaced fracture, and type 2 is a displaced fractures, with >1 mm displacement for fractures of the greater trochanter and >2 mm displacement for fractures of the lesser trochanter (see image below).
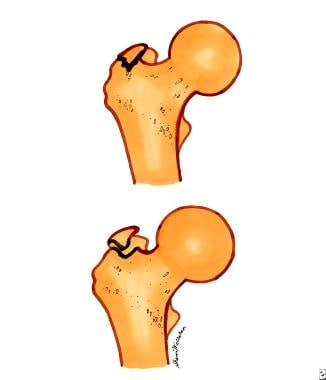 Trochanteric fractures. Top diagram is a nondisplaced trochanteric fracture. Bottom diagram is a displaced trochanteric fracture.
Trochanteric fractures. Top diagram is a nondisplaced trochanteric fracture. Bottom diagram is a displaced trochanteric fracture.
Intertrochanteric fractures
Intertrochanteric fractures are extracapsular fractures that occur in a line between the greater and lesser trochanters, generally in elderly patients and in women secondary to osteoporosis. Type 1 is a single fracture line without displacement and is stable; type 2 has multiple fracture lines (comminution) with displacement and is unstable (see image below).
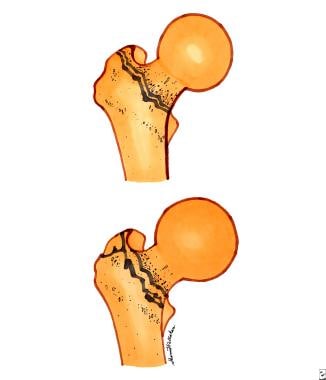 Intertrochanteric fractures. Top diagram is a single fracture line intertrochanteric fracture. Bottom diagram is a displaced, or multiple fracture line, intertrochanteric fracture.
Intertrochanteric fractures. Top diagram is a single fracture line intertrochanteric fracture. Bottom diagram is a displaced, or multiple fracture line, intertrochanteric fracture.
Subtrochanteric fractures
Subtrochanteric fractures have a bimodal age distribution and are seen most often in those aged 20-40 years, in association with high-energy trauma, and in patients older than 60 years secondary to falls on osteoporotic bones. It may be stable (bony contact of medial and posterior femoral cortices) or unstable.
Etiology
In young persons, hip fractures generally result from trauma associated with significant force. For example, 75% of all femoral head fractures, more common among young patients, occur as a result of motor vehicle collisions.
In older persons, more than 90% of hip fractures result from trauma or torsion associated with a minor fall or, occasionally, in the absence of any obvious traumatic event.
Risk factors
Osteoporosis is the leading cause of hip fracture. Digital x-ray radiogrammetry (DXR) of hand or wrist radiographs predicted hip fracture risk in a study of 5420 women and 2837 men. Bone mineral density equivalent, calculated from DXR, was significantly lower in the 122 patients who later suffered a hip fracture than in the patients who did not experience a hip fracture. The age-adjusted hazard ratio per standard deviation change in DXR score for hip fracture in the study was 2.52 and 2.08 for women and men, respectively. [1]
Additionally, Sennerby et al identified generalized cardiovascular disease as a significant risk factor for hip fracture, [2] and Carbone et al determined that heart failure increases hip fracture risk. [3] In men, smoking, tall stature, stroke, and dementia were found to increase the risk of hip fracture, whereas non–work-related physical activity and high body mass index (BMI) were protective. [4] A study found that previously elite male athletes sustained hip fractures at significantly older ages than their less active counterparts. [5]
Two medication classes have been implicated in hip fractures. Nursing home patients receiving antipsychotic medications and HIV-positive patients receiving protease inhibitor therapy were more likely to sustain fractures than those receiving other agents. [6, 7]
Other risk factors for hip fracture include the following:
-
Neurologic impairment
-
White race
-
Institutional living
-
Maternal history of hip fracture
-
Previous hip fracture
-
Physical inactivity
-
Alcohol abuse
-
Previous Colles or vertebral fracture attributed to osteoporosis
-
Low body weight
-
Impaired vision
-
Prolonged corticosteroid use
-
Use of medications that decrease bone mass, including furosemide, thyroid hormone, phenobarbital, and phenytoin
Egan et al identified several factors associated with the risk of a patient with hip fracture sustaining a second fall. [8] Increasing age, cognitive impairment, decreasing bone mass, decreasing depth perception, decreased mobility, dizziness, and a poor/fair self-perceived state of health were all linked to an increasing likelihood of sustaining a second fall and thus a possible second hip fracture.
Epidemiology
United States statistics
In the United States, hip fracture occurs in approximately 341,000 persons each year. [9] The US frequency of hip fracture, when age and sex are adjusted, ranks among the highest in the world.
International statistics
Western Europe and New Zealand also have reported high rates, with the lowest rates occurring in the South African Bantu people and in East Asian countries, where the incidence of osteoporosis is low. In North America and Europe, the rate of hip fracture is approximately 150 per 100,000 persons.
A study in Denmark reported that the incidence of hip fracture among patients aged 80 years and older has decreased by 35-40% during recent decades. [10] Similarly, an international study found that incidence rates declined in most countries from 2005-2018. [11]
Race-, sex-, and age-related demographics
The incidence of hip fracture is 2-3 times greater in Whites than in non-Whites, primarily because of the increased rate of osteoporosis in Whites. This difference is not unique to females; African American and Asian men have been found to have significantly higher bone densities than their White and Latino counterparts. [12]
Rate of hip fracture is 2-3 times greater in women than in men. At least 75% of all hip fractures occur in women. The lifetime risk of hip fracture in White women and men is 15% and 5%, respectively. Femoral neck fractures are more common in women than in men by about 4:1, while intertrochanteric fractures are more common in women than in men by about 5:1.
The rate of hip fracture increases with age, doubling every 5-6 years after age 60 years. The fracture rate does decrease slightly after age 85 years. [9] Nearly half of all hip fractures occur in adults older than 80 years. Hip fracture at a young age is rare and is usually the result of a high-velocity injury or, rarely, secondary to bone pathology.
Prognosis
Hip fracture outcomes vary considerably depending upon the patient's age, comorbidities, fracture type, and numerous other factors.
In general, young patients almost always regain the ability to ambulate, yet depending on fracture type, they may not return to their previous level of activity.
Many older patients do not regain the ability to ambulate or are able to do so only with assistance. This profoundly affects their ability to live independently.
Almost 20% of patients never regain the ability to ambulate, and a similar percentage are unable to ambulate outside their homes. Only 50-65% regain their premorbid ambulatory status.
The rate of recurrent injury in elderly patients with isolated hip fracture can be very high. Cabalatungan et al found that the rate of trauma-related recidivism in patients aged 65 years or older with hip fracture was 8.9% (87 of 974). The majority of patients with hip fracture were women (first injury, 74.7%; second injury, 66.5%). Low-level fall was the most common cause of injury (95.4%). [13]
Morbidity/mortality
Mortality
The reported overall mortality rate of hip fractures is 15-20%, yet in older persons this rate can increase to 36% over the year following hip fracture. Rate of mortality is greatest in the first few months following injury but remains high for up to 1 year. It then returns to the same rate for age- and sex-matched people without hip fracture. [14]
Surgical delay independently affects mortality. Patients for whom surgery is delayed for 2 days or more have a 17% higher mortality at 1 month. A subsequent study showed increased mortality but decreased readmission rate in those in whom repair was done more than 4 days after injury. [15] Also, general anesthesia was associated with higher morbidity than was spinal/epidural anesthesia.
In a Swedish study by Ioannidis et al, hip fracture patients with dementia had a higher risk of death in the first 30 days after surgery. The adjusted risk of all-cause 30-day postoperative mortality was 67% higher in patients with dementia than in patients without dementia. Patients with dementia had a sevenfold increased risk of cerebrovascular-associated mortality. [16]
In a German prospective study by Knauf et al, 5-year survival of patients 60 years or older with hip fracture was 38% (152/395). Risk factors included older age, lower Mini-Mental State Examination, and the presence of delirium during hospitalization. [17]
Morbidity
Morbidity associated with hip fracture is staggering, especially in older persons. Morbidity from immobilization includes development of deep vein thrombosis, pulmonary embolism, pneumonia, and muscular deconditioning. Morbidity from surgical procedures includes complications of anesthesia, postoperative infection, loss of fixation, and malunion or nonunion, as well as the complications associated with immobilization. As many as 20% of patients return to the emergency department in the year following a hip fracture with concerns relating to morbidity associated with the initial fracture. [18]
Surgical delay of more than 48 hours has been shown to increase morbidity as well as mortality. [19]
Hip fracture resulting from major trauma often is associated with other bone and soft-tissue injuries, intra-abdominal and intrapelvic injuries, major blood loss, head and neck injuries, and other extremity injuries. Morbidity associated with an inability to return to a prefracture level of mobility results in a loss of independence, reduction in quality of life, and depression, particularly in older persons.
Complications
Complications associated with hip fracture include the following [20, 21] :
-
Delirium: 13.5-33%
-
Pulmonary embolism: 1.4-7.5%
-
Deep venous thrombosis: 27%
-
Pneumonia: 7%
-
Myocardial infarction or heart failure: 35-42%
-
Urinary retention or infection: 12-61%
-
Acute kidney injury: 11%
-
Anemia: 24-44%
-
Skin pressure damage: 7-9%
-
Shenton line and angular anatomy of the femur.
-
Femoral head fractures. Top diagram is a single-fragment femoral head fracture. Bottom diagram is a comminuted femoral head fracture.
-
Femoral neck fractures. Top diagram is a nondisplaced, or incomplete, femoral neck fracture. Bottom diagram is an impacted femoral neck fracture.
-
Partially displaced femoral neck fracture.
-
Completely displaced femoral neck fracture.
-
Trochanteric fractures. Top diagram is a nondisplaced trochanteric fracture. Bottom diagram is a displaced trochanteric fracture.
-
Intertrochanteric fractures. Top diagram is a single fracture line intertrochanteric fracture. Bottom diagram is a displaced, or multiple fracture line, intertrochanteric fracture.