Background
Polymorphic eruption of pregnancy (PEP), first described as pruritic urticarial papules and plaques of pregnancy (PUPPP), refers to a benign dermatosis that usually arises late in the third trimester of a first pregnancy. [1, 2] It can also manifest immediately postpartum. [3] The entity previously had been reported as toxemic rash of pregnancy, [4] toxemic erythema of pregnancy, and late-onset prurigo of pregnancy. See the image below.
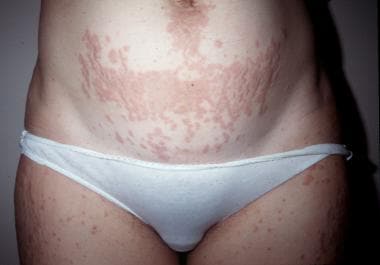 Papules within prominent striae distensae. Courtesy of Jeffrey P. Callen, MD of Louisville, Kentucky.
Papules within prominent striae distensae. Courtesy of Jeffrey P. Callen, MD of Louisville, Kentucky.
Following atopic eruption of pregnancy, which occurs earlier in gestation, PEP is the second most common pruritic dermatosis of pregnancy. [5] One European author proposes that early gestational papular dermatoses (usually atopic eruption of pregnancy) be referred to as "early-onset PEP," distinguished from "late-onset PEP". [6]
Epidemiology
Polymorphic eruption of pregnancy (PEP) occurs in 1 out of 160 pregnancies. [6, 7] The condition may be less common in Blacks.
Etiology
The cause and pathogenesis of polymorphic eruption of pregnancy (PEP) are not known. A meta-analysis revealed that 11.7% of patients with PEP had multiple gestation pregnancies. [8] Within that group, a higher PEP risk for triplet (14%) over twin (2.9%) pregnancies was found, [9] suggesting a relationship between skin distention and the development of PEP. Most studies have revealed increased maternal weight gain in patients with PEP when compared with normal pregnancies, further supporting the role of increased skin distention. [2, 7, 10]
A study from Israel also found maternal hypertension and induction of labor to be significantly associated with the condition. [11] One large series of cases revealed a male-to-female infant ratio of 2:1. [12]
Investigators identified fetal deoxyribonucleic acid (DNA) in the skin of mothers with PEP, suggesting that chimerism may be relevant to the pathogenesis of this disorder. [13] Additionally, another suggested cause is the maternal immune reaction to the fetal antigens within the maternal bloodstream. [14] Finally, a case-control study from France confirmed previously documented associations with multiple gestations, cesarean deliveries, and male fetuses, although no relationship to maternal or fetal weight gain was noted. [15]
One case report identifies PEP that occurred simultaneously with COVID-19 symptoms, such as fever, headache and diarrhea, in the postpartum period. This association could suggest that SARS-CoV-2 plays a role in the pathogenesis of PEP. [16]
Another case reports a coexistence of PEP superimposed on junctional epidermolysis bullosa. The patient likely had PEP, and the pruritus caused her to scratch, leading to bullae and erosions. [17]
A study from Japan found that the development of PEP may be linked to an immune response characterized by an increased activity of Th2 cytokines, such as interleukin 33 (IL-33) and IL-9. [18]
Another study from Turkey indicated that PEP was more common in in vitro fertilization (IVF) pregnancies than in spontaneous pregnancies, even in singleton pregnancies. Similarly, increased doses of progesterone or prolonged use of progesterone may contribute to the pathogenesis of PEP. [19]
Prognosis
The prognoses for the affected patient and the newborn are excellent in polymorphic eruption of pregnancy (PEP). It typically resolves within 4-6 weeks, independent of delivery, [7] and the condition does not tend to recur in subsequent pregnancies. Only 7% of multiparous PEP patients described a similar rash with prior pregnancies. [5] Patients who have had PEP will not precipitate a return of the condition through the subsequent use of oral contraceptives.
No mortality is associated with PEP. The mere appearance of an unusual skin eruption in pregnancy can provoke anxiety, but the pruritus is the most distressing feature. The later weeks of pregnancy can be associated with many physical symptoms, and the severe itching of PEP may further debilitate and aggravate sleep loss in the weeks prior to delivery. No known systemic complications exist for affected patients, and fetal mortality or morbidity does not increase.
Patient Education
The patient should understand that PEP is a benign disorder and has not been shown to have adverse consequences for the fetus. Fully explain the side effects of corticosteroids and antihistamines (which are used in the treatment of PEP). Reassure the affected patient that PEP does not usually recur with subsequent pregnancies and will not be triggered by future use of oral contraceptives.
-
Papules within prominent striae distensae. Courtesy of Jeffrey P. Callen, MD of Louisville, Kentucky.
-
Papules within prominent striae distensae. Courtesy of Jeffrey P. Callen, MD of Louisville, Kentucky.

