Background
Blue rubber bleb nevus syndrome (BRBNS) is a rare condition that is characterized by numerous malformations of the venous system that significantly involve the skin and visceral organs. [1] This condition was initially discovered in 1860 by Gascoyen. [1] However, it was later made famous in 1958, by William Bennett Bean for which the disease has been termed "bean syndrome," later referenced as blue rubber bleb nevus syndrome. [1] BRBNS is an important condition due to the potential for significant bleeding which can be fatal.
Also see the article, Dermatologic Manifestations of Gastrointestinal Disease.
Note the images below.
Pathophysiology
Skin manifestations can typically be found at birth, whereas, organ system involvement tends to appear later in life. [1] The internal organ system most frequently involved is the GI system, for which GI bleeding is a common symptom. [2] Therefore, GI bleeding can lead to anemia and severe cases of hemorrhage may require transfusion therapy. [2] Additional complications include telescoping of the intestines, volvulus, and necrosis of the intestinal mucosa. [3] In addition, multiple vascular blebs and nodules can be found throughout the body. Case reports have demonstrated involvement of the CNS, thyroid, parotid, eyes, oral cavity, musculoskeletal, oral cavity, lungs, liver, spleen, and bladder. Although, literature suggests the coexistence of CNS with GI symptoms, they are still rare. [3]
Histopathologic examination of the lesions will reveal ecstatic vascular dilated spaces filled with endothelial cells forming a single layer, surrounded by connective tissue. [4]
Etiology
The etiology of blue rubber bleb nevus syndrome (BRBNS) remains unknown. [5] The literature suggests that this condition occurs sporadically. [5, 6] A few reported cases have been associated with an autosomal dominant inheritance pattern, for which a locus was found on chromosome 9p. [5, 7] One case report of BRBNS was discovered to be associated with pancreatic lymphangiomas. The systemic vascular lesions found in that case were linked to a familial germ line functional mutation (Arg849Trp) in the TIE2 gene. [8]
Epidemiology
Frequency
Blue rubber bleb nevus syndrome (BRBNS) is a rare condition with about 200 cases reported in the literature. [6]
Race
Blue rubber bleb nevus syndrome (BRBNS) has been reported to occur in people of all races; [9] however, whites appear to be most frequently affected.
Sex
Blue rubber bleb nevus syndrome (BRBNS) affects both males and females equally. [3, 6]
Age
Skin manifestations of blue rubber bleb nevus syndrome (BRBNS) typically can be present at birth or evident in early childhood. [1] Visceral organ involvement tends to appear later in life, traditionally around early adulthood. [1]
Prognosis
The prognosis for blue rubber bleb nevus syndrome (BRBNS) depends on the extent of visceral organ involvement and complications related to the degree of symptoms. Most patients are expected have a normal life span.
The morbidity related to this condition depends on the extent of GI involvement, ranging from minimal to invasive. [1, 10] To date the literature supports no evidence of a carcinogenetic or fatal conversion of this condition. [10] Therefore, the malignancy potential has not yet been determined. [10] A complication of this condition is profound GI hemorrhage, which can lead to death. [1, 10] Serial transfusions and periodic surveillance can modify the morbidity of the disease. Lesions involving bones and joints can cause profound discomfort and loss of function, requiring amputations in some cases. Rarely, CNS involvement can be fatal. [11]
-
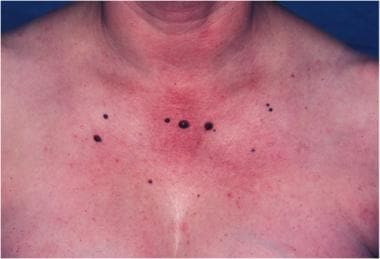
Multiple scattered blue to black rubbery papules and nodules involving the mid-chest region.
-
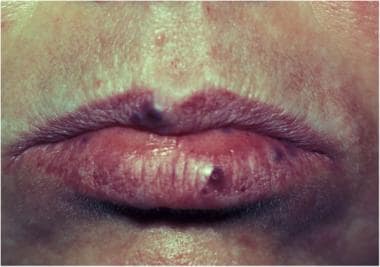
Purple to blue/black papules involving the upper and lower lips.
-
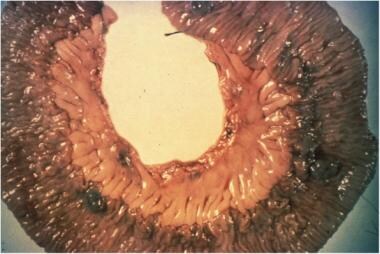
Multiple blue to black pigmented, rubbery, blood-filled sacs, which are easily compressible involving the GI tract.
-
Lower extremity cutaneous lesions described in blue rubber bleb nevus syndrome, consisting of blue rubbery papules and nodules with an easily compressible smooth surface.
-
Histopathology reveals blood-filled vessels, composed of single layers of endothelium, surrounded by connective tissue.