Overview
The eyelids act to protect the anterior surface of the globe from local injury. Additionally, they aid in the regulation of light reaching the eye. In tear film maintenance, eyelids are responsible for distributing the protective and optically important tear film over the cornea during blinking. In tear flow, eyelids are involved in in a pumping action on the conjunctival sac and lacrimal sac.
Structures that must be considered in a description of lid anatomy are [1]
The skin and subcutaneous tissue: The outermost layer that provides protection and houses glands.
The orbicularis oculi muscle (shown below): This sphincter-like muscle encircles the eyelids, enabling closure and contributing to blinking. It consists of two parts: the orbital section for forceful closure and the palpebral section (further divided into preseptal and pretarsal components) for gentle blinking.
The submuscular areolar tissue : A loose connective tissue layer that allows flexibility and movement.
The fibrous layer: This layer comprises the tarsal plates (which provide structural support) and the orbital septum (the anatomical boundary between eyelid tissues and orbital tissues).
The lid retractors of the upper and lower eyelids: These include the levator palpebrae superioris and Muller muscle in the upper eyelid and the capsulopalpebral fascia in the lower eyelid, which are responsible for elevating the eyelids.
The retroseptal fat pads: Fat deposits that cushion and support the eyelids
The conjunctiva: A mucous membrane that lines the inside of the eyelids and covers the sclera, playing a role in tear production and eye protection
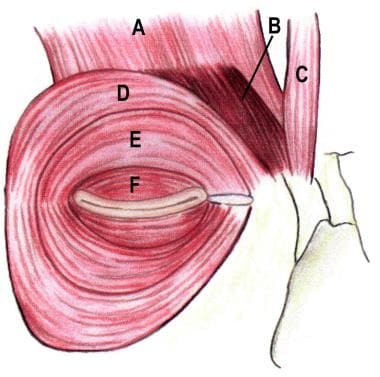 Orbicularis oculi muscle anatomy. (A) Frontalis, (B) corrugator superciliaris, (C) procerus, (D) orbital orbicularis, (E) preseptal orbicularis, (F) pretarsal orbicularis.
Orbicularis oculi muscle anatomy. (A) Frontalis, (B) corrugator superciliaris, (C) procerus, (D) orbital orbicularis, (E) preseptal orbicularis, (F) pretarsal orbicularis.
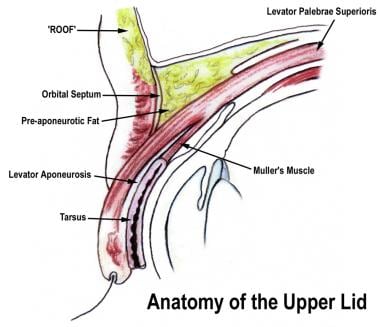
The anatomy of the lid is best approached initially by reviewing a sagittal cross section of the eyelid. The exact number of tissue layers and the relationship between the many layers are modified significantly by the level of the lid examined. The orbital septum represents the anatomic boundary between the lid tissue and the orbital tissue, but the assessment of eyelid function and preparation for lid surgery require knowledge of these postseptal structures. The upper and lower lids may be considered analogous structures, with differences mainly in the lid retractor arrangement. [2]
In eyelid reconstruction, it is more practical to consider the repair of the anterior and posterior lamellae, with the anterior lamella being the skin and orbicularis and the posterior lamella being the tarsus and conjunctiva.
For patient education information, see the Eye and Vision Center, as well as Anatomy of the Eye.
Surface Anatomy
The upper eyelid extends superiorly to the eyebrow, which separates it from the forehead. The lower lid extends below the inferior orbital rim to join the cheek, forming folds where the loose connective tissue of the eyelid is juxtaposed with the denser tissue of the cheek (see the images below).
The upper eyelid skin crease (superior palpebral sulcus) is approximately 8-11 mm superior to the eyelid margin and is formed by the attachment of the superficial insertion of levator aponeurotic fibers (8-9 mm in men and 9-11 mm in women). The inferior eyelid fold (inferior palpebral sulcus), which is seen more frequently in children, runs from 3 mm inferior to the medial lower lid margin to 5 mm inferior to the lateral lid margin.
The nasojugal fold runs inferiorly and laterally from the inner canthal region along the depression of separation of the orbicularis oculi and the levator labii superioris, forming the tear trough. The malar fold runs inferiorly and medially from the outer canthus toward the inferior aspect of the nasojugal fold.
The open eye presents the palpebral fissure, a fusiform space between the lid margins that is 28-30 mm in length and about 9 mm in maximal height. The lid margins join at their extremities, forming the medial and lateral canthus. [1] The natural curvature of the upper lid is a function of the static shape of the tarsus combined with adaptation of the lid to the curvature of the globe.
In the normal adult fissure, the highest point of the upper lid is just nasal to the center of the pupil, while the lowest point of the lower lid is just temporal to the center of the pupil. In youths, the upper lid margin rests at the upper limbus, while in adults, it rests 1.5 mm below the limbus. The lower eyelid margin rests at the level of the lower limbus. The lateral canthal angle is 2 mm higher than the medial canthal angle in Europeans; it is 3 mm higher in Asians. The distance from the medial canthus to the midline of the nose is approximately 15 mm (see the image below).
The palpebral fissure presents the lateral canthus (an angle of 30-40° approximately 5 mm from the lateral orbital rim), the medial canthus (forming the medial angle of the fissure, with the upper border passing inferomedially and the lower border passing horizontally), and the lacrimal papillae, which rest on the free lid margin, with the punctum lacrimale serving as an opening to the canaliculus.
The arterial supply to both eyelids arises from the branches of the ophthalmic artery. The upper eyelid receives blood primarily from the medial and lateral palpebral branches, while lymphatic drainage occurs through the parotid and submandibular nodes. Sensory innervation is provided by branches of both the ophthalmic (CN V1) and maxillary (CN V2) divisions of the trigeminal nerve. [1, 3]
Skin and Subcutaneous Tissue
The skin of the eyelids is the thinnest of the body (< 1 mm). This delicate skin is crucial for protecting the eye while also facilitating various functions related to vision and tear distribution. [1] The upper eyelid contains a delicate connective tissue layer beneath its skin surface. [1, 4]
The nasal portion of the eyelid skin has finer hairs and more sebaceous glands than the temporal aspect, making this skin smoother and oilier. The transition from this thin eyelid skin to the thicker skin of the eyebrow (approximately 10 mm below the lower eyebrow hairs) and the cheek skin (below the nasojugal and malar folds) is clinically evident. These boundaries should be considered in reconstructive eyelid surgery. The subcutaneous tissue consists of loose connective tissue.
Fat is very sparse in preseptal and preorbital skin and is absent from pretarsal skin. Subcutaneous tissue is absent over the medial and lateral palpebral ligaments, where the skin adheres to the underlying fibrous tissue. The subcutaneous layer's composition allows for flexibility and movement while providing minimal cushioning, which is essential for eyelid function. [1]
Dermatochalasis, blepharochalasis, and epicanthic folds all are conditions that primarily involve the skin and subcutaneous tissue of the eyelids.
An in-depth understanding of the eyelid anatomy is crucial for effective surgical planning and minimizing complications during procedures such as eyelid reconstruction. Techniques such as local random flaps or grafts are often utilized to restore both function and appearance following defects or trauma. [5]
Orbicularis Oculi Muscle
The orbicularis oculi muscle is one of the superficial muscles of facial expression. Invested by the superficial musculoaponeurotic system (SMAS), muscle contracture is translated into movement of the overlying tissues by the fibrous septa extending from the SMAS into the dermis.
The orbicularis oculi can be categorized into three main parts: orbital, palpebral, and lacrimal (deep palpebral). [1]
The orbital portion extends in a wide, circular fashion around the orbit, interdigitating with other muscles of facial expression. It has a curved origin from the medial orbital margin, being attached to the superomedial orbital margin, maxillary process of the frontal bone, medial palpebral ligament, frontal process of the maxilla, and inferomedial orbital margin.
Fibers from this medial origin sweep around the orbital margin in a horseshoe fashion. The muscle fibers extend superiorly to intermix with the frontalis muscle and corrugator supercilii muscle, laterally to cover the anterior temporalis fascia, and inferiorly to cover the origins of the lip elevators.
The palpebral part is further divided into the marginal, pretarsal, and preseptal parts. [1]
The preseptal orbicularis muscles overlie the orbital septum and originate medially from a superficial and deep head associated with the medial palpebral ligament. The fibers from the upper and lower lid join laterally to form the lateral palpebral raphe, which is attached to the overlying skin.
The pretarsal portion lies anterior to the tarsus, with a superficial and deep head of origin intimately associated with the medial palpebral ligament. Fibers run horizontally and laterally to run deep to the lateral palpebral raphe to insert in the lateral orbital tubercle through the intermediary of the lateral canthal tendon (LCT).
The palpebral portion is used in blinking and voluntary winking, while the orbital portion is used in forced closure.
The lacrimal part originates from the posterior lacrimal crest of the lacrimal bone as well as from the medial palpebral ligament. Its fibers primarily insert into the lateral palpebral raphe, where they blend with adjacent muscle fibers and contribute to the overall structure of the eyelids. The lacrimal part compresses the lacrimal sac during blinking, which helps to facilitate tear drainage. This action creates a negative pressure within the sac, allowing tears to flow from the eye surface into the nasolacrimal duct. By drawing the eyelids medially, this portion aids in ensuring that tears are effectively distributed across the ocular surface, enhancing lubrication and protection against foreign particles. This muscle's interaction with the nasolacrimal duct system is vital for maintaining proper tear film stability and eye health. When functioning correctly, it ensures that tears are efficiently drained from the eye, preventing overflow, and maintaining moisture levels. [1]
Facial nerve innervation is from the temporal branches and zygomatic branches of the facial nerve. The nerves are orientated horizontally and innervate the muscle from the undersurface.
Studies have also highlighted an intricate relationship between the orbicularis oculi and surrounding musculature, particularly how fibers from adjacent muscles such as the frontalis interconnect with it. This anatomical interplay contributes significantly to facial expressions and overall aesthetic appearance. [6]
Submuscular Areolar Tissue
Submuscular areolar tissue consists of variable, loose connective tissue below the orbicularis oculi muscle. The lid may be split into anterior and posterior portions through this potential plane, which is reached by division at the gray line of the lid margin.
In the upper lid, this plane is traversed by fibers of the levator aponeurosis, some of which pass through the orbicularis to attach to the skin to form the lid crease. In the lower eyelid, this plane is traversed by fibers of the orbitomalar ligament, also called the orbicularis retaining ligament. This ligament connects the orbicularis oculi muscle to the lower orbital rim and plays a role in maintaining eyelid structure and function. [1]
Superior continuance in this submuscular plane arrives at the retro-orbicularis oculi fat (ROOF), which is best developed in the eyebrow region. Additionally, the suborbicularis oculi fat (SOOF) is found in the lower lid in continuance with this plane.
The ROOF and SOOF are critical in maintaining the shape and function of the eyelid, as well as in aesthetic considerations. The integrity of this tissue layer is crucial as it supports the skin and muscle, influencing both functional movement and the appearance of the eyelids, especially with aging. [1]
Tarsi and Orbital Septum
Tarsal plates
The tarsal plates are composed of dense fibrous tissue and are responsible for the structural integrity of the lids. Each tarsus is approximately 29 mm long and 1 mm thick. The crescentic superior tarsus has a vertical height of 10 mm centrally, narrowing medially and laterally. The lower border of the superior tarsus forms the posterior lid margin. The rectangular inferior tarsus is 3.5-5 mm high at the eyelid center. The posterior surfaces of the tarsi adhere to the conjunctivae.
Immunohistochemical studies suggest that the tarsus exhibits characteristics of both dense fibrous connective tissue and cartilage, containing fibroblasts within an extracellular matrix rich in type I and III collagen, alongside proteoglycans. [7]
Each tarsus encloses about 25 sebaceous meibomian glands, which span the vertical height of the tarsus. Their ducts open at the lid margin posterior to the grey line and just anterior to the mucocutaneous junction. These glands are crucial for maintaining tear film stability and preventing dry eye syndrome. [8]
The medial and lateral ends of the tarsi are attached to the orbital rims by the medial and lateral palpebral ligaments.
Medial palpebral ligament
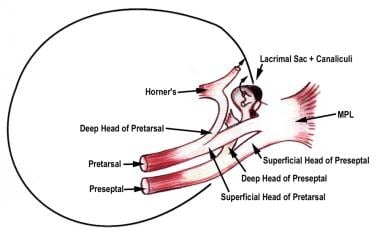
The medial palpebral ligament (medial canthal tendon [MCT]) is a fibrous band that stabilizes the medial tarsi and is intricately related to the orbicularis oculi muscle and the lacrimal system. The superficial head of the pretarsal orbicularis muscle lies anterior to the canaliculi and forms the anterior limb of the MCT. This head is primarily horizontal but also has a superior supporting extension inserting onto the frontal bone. The deep head of the pretarsal orbicularis muscle (also constituting the Horner muscle) inserts into the posterior lacrimal crest and onto the fascia of the lacrimal sac.
The upper and lower lid preseptal orbicularis have a superficial head that inserts into and augments the MCT and deep heads that insert into the lacrimal sac fascia. Thus, the lacrimal sac, encased in fascia, is related anteriorly, laterally, and posteriorly to the constituents of the MCT and medially to the bony fossa of the lacrimal sac (see the image below).
Lateral palpebral ligament
The lateral palpebral ligament (lateral canthal tendon [LCT]) is formed by dense fibrous tissue arising from the tarsi and passes laterally deep to the septum orbitale to insert into the lateral orbital tubercle 1.5 mm posterior to the lateral orbital rim. The tendon is approximately 10.5 mm in length and 6.5 mm in width, and the midpoint of the LCT inserts 10 mm inferior to the frontozygomatic suture. The LCT lies beneath the orbital septum and the lateral palpebral raphe of orbicularis oculi. Thus, it is situated more deeply in comparison with the MCT. [11] A small pocket of fat (Eisler pocket) lies between the septum and the LCT. The LCT is also attached to the lateral orbital rim more superficially through the orbital septum. This superficial fascial plane has been characterized by Knize as the "superficial LCT" and may be used as a structure to suspend or stabilize the lateral canthus. [9]
Superiorly, the LCT is contiguous with the lateral horn of the levator aponeurosis, while the inferior edge is well defined and arcs inferiorly to its insertion. About 2 mm of lateral movement of the lateral canthal angle occurs during abduction, presumably caused by posterior fibrous attachments to the lateral check ligament of the lateral rectus muscle.
Flowers et al described a lateral tarsal strap, distinct from the LCT, as a broad and strong structure connecting the lower lid tarsal plate to the inferolateral orbital rim. [10] The tarsal strap attaches 3 mm inferiorly and 1 mm deep to the LCT, approximately 4-5 mm deep to the anterior orbital rim. Upon surgical release of the tarsal strap, the lateral canthus is elevated easily.
Studies emphasize that both tarsal plates work in concert with the surrounding muscles, including the levator palpebrae superioris, which elevates the upper eyelid. The superior tarsal muscle (Müller's muscle), an accessory smooth muscle, also contributes to eyelid elevation by providing additional lift beyond that achieved by contraction of the levator palpebrae superioris. [11]
Orbital septum
The orbital septum is a connective tissue structure that attaches peripherally at the periosteum of the orbital margin (the arcus marginalis); it centrally fuses with the lid retractor structures near the lid margins, thus acting as a diaphragm (that has been reported to retain orbital contents). Although usually depicted diagrammatically as a discrete layer immediately posterior to the orbicularis oculi muscle, the orbital septum is a multilaminated structure that is part of the anterior orbital connective tissue framework. The septum has a laxity consistent with the mobility of the eyelids.
Laterally, the septum is attached to the orbital margin, 1.5 mm in front of the lateral orbital tubercle attachment of the lateral palpebral ligament. The Eisler fat pocket separates the lateral palpebral ligament from the orbital septum. From there, the septum continues along the superior orbital rim at the arcus marginalis. Superomedially, the septum bridges the supraorbital groove, passes inferomedially anterior to the trochlea, and then follows the posterior lacrimal crest. As it runs down the posterior lacrimal crest, it lies anterior to the medial check ligament and posterior to the Horner muscle (and hence behind the lacrimal sac).
The line of attachment crosses the lacrimal sac fascia to reach the anterior lacrimal crest at the level of the lacrimal tubercle. From there, it passes inferiorly down the anterior lacrimal crest and laterally along the inferior orbital rim. A few millimeters lateral to the zygomaticomaxillary suture, the attachment leaves the rim and lies several millimeters from it on the facial aspect of the zygomatic bone, thus forming the fat-filled premarginal recess of Eisler. The line of attachment then continues to again reach the lateral orbital rim, just below the level of the Whitnall ligament.
Reid et al proposed the existence of a septal extension, from the line of fusion of the orbital septum to the levator aponeurosis, extending caudally to cover the tarsal plate up to the ciliary margin. [12] The septal extension acts as an adjunct to the levator aponeurosis; identifying this structure may be important to avoid relapse or complications in ptosis repair and blepharoplasty.
The orbicularis retaining ligament
The orbicularis retaining ligament (also called the orbitomalar ligament or the orbicularis retaining septum) attaches the orbicularis oculi to the inferior orbital rim; it is broader and stronger inferolaterally than centrally. This ligament is a bilaminar membrane separated by a thin layer or fat along the inferior orbital rim and spans circumferentially around the entire orbit. The expanded lateral end of the orbicularis retaining ligament is continuous with the lateral orbital thickening. The orbicularis retaining ligament ends medially with direct connection to the orbicularis oculi muscle approximately at the level of the nasal limbus, above the levator labii superioris. It has been shown to be consistently inferior to the zygomaticofacial nerve and foramen, making it an important surgical landmark. [13] The orbicularis retaining ligament is distinct from the orbital septum, and the two fuse to form the arcus marginalis.
Orbital thickening is a fibrous fusion between the orbicularis fascia covering the peripheral part of the orbicularis oculi and the underlying deep fascia (i.e., periosteum and the deep temporalis fascia). This thickening extends across the entire width of the frontal process of zygomatic bone and onto the deep temporal fascia for a variable distance, marking a vital surgical landmark. [1]
With age, the retaining ligament becomes thin and distended, with the changes being greater centrally than laterally. During surgery, detachment of the orbital thickening and the lateral part of the retaining ligament completely releases the superficial fascia from the orbital rim.
Observations on aging indicate that changes in fat distribution within the eyelids can lead to alterations in septal structure and function. Specifically, herniation of the orbital fat can compress areas of the orbital septum, affecting surgical approaches and outcomes in aesthetic procedures. [14]
The orbital septal flap has emerged as a reliable method for managing conditions such as upper eyelid retraction. A study involving 46 eyes of 43 consecutive patients with moderate or severe upper eyelid retraction showed significant improvement in eyelid position after surgery using this flap technique. [15]
Eyelid Retractors
Upper lid retractors
The levator palpebra superioris (LPS) arises at the orbital apex from the undersurface of the lesser wing of the sphenoid bone. The levator muscle and the superior rectus muscle share a developmental origin and are connected by fibrous attachments. The LPS proceeds anteriorly for 40 mm and ends in an aponeurosis approximately 10 mm behind the orbital septum. The levator complex changes direction from a horizontal to a more vertical direction at the superior transverse ligament (Whitnall ligament).
The superior transverse ligament lies near the junction of the muscular and aponeurotic levator and represents an orbital fascial condensation spanning the anterosuperior orbit between the trochlea and the lacrimal gland fascia. Variations in thickness and adherence to the levator complex are evident. Thin fascial attachments lie between the superior transverse ligament and the superior orbital rim.
The levator aponeurosis spreads laterally and medially to form lateral and medial horns. The medial horn attaches to the posterior lacrimal crest. The lateral horn divides the lacrimal gland into orbital and palpebral lobes before attaching to the lateral retinaculum at the lateral orbital tubercle. The aponeurosis fuses with the orbital septum prior to reaching the level of the superior tarsal plate border. At the inferior edge of this fusion, some aponeurotic fibers descend to insert into the lower third of the anterior surface of the tarsal plate. An anterior extension from this fusion inserts into the pretarsal orbicularis oculi muscle and overlying skin, forming the upper lid skin crease.
Kakizaki proposed that the levator aponeurosis consists of two layers, anterior and posterior, which also contain smooth muscle in their proximal parts. [16] The anterior layer ends in the junctional region with the orbital septum and pulls the preaponeurotic pad of fat in conjunction with the orbital septum and the submuscular fibroadipose tissue. The posterior layer is attached to the anterior inferior one third of the tarsal plate. It thus regulates the tension of the eyelid and the ordered movement of the lid.
Müller's muscle is a smooth muscle innervated by the sympathetic nervous system. Fibers originate from the undersurface of the levator in the region of the aponeurotic muscle junction, travel inferiorly between the levator aponeurosis and conjunctiva, and insert into the superior margin of the tarsus. With age, fatty infiltration may occur, giving the muscle a yellowish color.
Müller's muscle plays a significant role in eyelid retraction; notably, it has been identified as having proprioceptive functions, suggesting that it contributes to eyelid spatial positioning and retraction. [17]
Contrary to previous understanding, Müller's muscle may also be involved in thyroid eye disease (TED) by fibrosis and mast cell infiltration. It may function as a large, serial muscle spindle. This function allows it to respond reflexively during eyelid movements, potentially maintaining visual fields by adjusting eyelid position. [18] The stretching of this muscle by the initial eye opening action of the levator may initiate a reflex via the mesencephalic trigeminal nucleus, which subsequently is routed through the ipsilateral or bilateral levator muscle, evoking involuntary tonic contraction to maintain an adequate visual field.
Surgical techniques have evolved for addressing eyelid retraction associated with conditions such as TED. Various approaches aim to debilitate both the levator muscle and Müller's muscle through anterior or posterior techniques. The posterior approach allows for correction without external scarring, preserving anterior eyelid structures for potential future interventions. Studies have reported high success rates for these surgical methods, emphasizing their effectiveness in managing upper eyelid retraction while minimizing complications. [18]
The peripheral vascular arcade of the upper eyelid lies adherent to the lower border of the anterior surface of the Müller's muscle, just above the upper border of the tarsus, and is apparent during blepharoptosis surgery as a plane of dissection is created between the levator aponeurosis and the Müller's muscle. The action is to widen the palpebral fissure with increased sympathetic tone. About 2 mm of ptosis is observed in patients with Horner syndrome. Sympathetically innervated smooth muscle fibers are also noted in the lower eyelid and constitute the inferior tarsal muscle.
Lower lid retractors
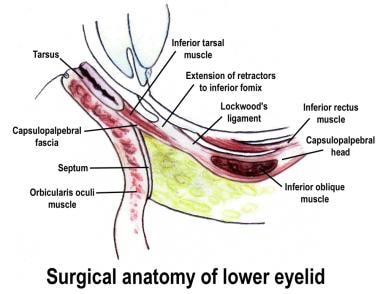
The lower eyelid retractor is a fascial extension from the terminal muscle fibers and tendon of the inferior rectus muscle, originating as the capsulopalpebral head. As it passes anteriorly from its origin, it splits to envelop the inferior oblique muscle and reunites as the inferior transverse ligament (Lockwood ligament). From there, the fascial tissue passes anterosuperiorly as the capsulopalpebral fascia. The bulk of the capsulopalpebral fascia inserts on the inferior border of the inferior tarsus. Fibers also pass forward, to unite with the Tenon capsule, and to the inferior fornix conjunctiva, through orbital fat to the orbital septum, and forward to the subcutaneous tissues forming the lower eyelid crease. The orbital septum fuses with the capsulopalpebral fascia approximately 5 mm below the inferior tarsal border.
The inferior tarsal muscle (Müller's muscle) lies just posterior to the fascia and is intimate with its structure. The sympathetically innervated smooth muscle fibers are first noted near the origin of the capsulopalpebral head. The capsulopalpebral head splits into two portions to pass around the inferior oblique muscle sheath; the portion beneath the muscle is thin and devoid of smooth muscle, while the portion above is a much thicker fascial layer and contains the smooth muscle fibers. As they continue to pass forward, the smooth muscle fibers do not insert directly onto the inferior tarsal border but into the fascia several millimeters below the tarsal border.
In the Asian lower lid, the line of fusion of the orbital septum to the capsulopalpebral fascia is often higher or indistinct, with anterior and superior orbital fat projection, and overriding of the preseptal orbicularis oculi over the pretarsal orbicularis. [19]
Surgical techniques such as posterior layer advancement of lower eyelid retractors with transcanthal canthopexy have shown promising outcomes for conditions such as involutional entropion. This technique has been associated with shorter surgical times and reduced risk for lateral canthal deformity compared to traditional methods. [20]
Combined procedures that address both orbital decompression and lower eyelid retraction have demonstrated significant improvements in eyelid positioning and patient satisfaction. This approach not only enhances aesthetic outcomes but also addresses functional issues such as dry eye symptoms. [21]
Fat Pads
The orbital fat of the upper eyelid is divided into two components: the preaponeurotic (central) fat pad and the medial fat pad. The upper eyelid preaponeurotic fat is found immediately posterior to the orbital septum and anterior to the levator aponeurosis. A central fat pad and a medial fat pad are described in the upper lid, while the lacrimal gland occupies the lateral compartment. The preaponeurotic fat pad is continuous with the deeper orbital fat, whereas, medially, the reflected tendon of the superior oblique and medial horn of the levator aponeurosis separate it from the medial fat pad. [22] The medial fat pad is usually pale yellow or white and lies anterior to the levator aponeurosis extending superomedial to the medial horn of the levator. The medial fat pad contains many plural divisions: the medial superior fat pad and medial inferior fat pad, half of which are delineated by delicate fibroareolar tissue. [22]
The central fat pad is yellow and broad. It can be recognized by its yellowish color due to a higher level of carotenoids. [23]
The medial fat pad may become more prominent over time as the central fat pad recedes with age-related changes, such as enophthalmos, where the eyeball appears sunken. [24]
A portion of the lateral end of this pad surrounds the medial aspect of the lacrimal gland. The lacrimal gland has a firm, pinkish, lobulated structure, in contrast to the soft, yellow intraorbital fat. The lacrimal gland's anterior border is normally just behind the orbital margin, but involutional changes may lead to prolapse anteroinferiorly, which is prominent on external lid examination.
Three retroseptal fat pads are associated with the lower eyelid. The medial and central fat pads are separated by the inferior oblique. However, an isthmus of fat generally lies anterior to the muscle belly. The inferior oblique muscle takes a bony origin from a shallow depression on the anteromedial orbital floor, directly posterior to the orbital margin and lateral to the nasolacrimal canal.
The inferior oblique muscle courses posterolaterally, passing inferior to the inferior rectus muscle, penetrating the Tenon capsule, and inserting onto the globe near the macula. Its course makes it susceptible to injury during surgical dissection of the surrounding fat pads.
The medial and lateral fat pads are separated by the arcuate expansion, a fascial band extending from the capsulopalpebral fascia to the inferolateral orbital rim. This anatomical arrangement is crucial for surgical interventions such as blepharoplasty, where preserving these compartments can prevent complications such as tear trough deformities. [25]
Notably, the inferolateral orbital septum is inserted 2 mm outside the orbital rim, creating the recess of Eisner, allowing the lateral fat pad to just spill over the orbital rim.
Studies indicate that lower eyelid fat pads are distinct from posterior intraorbital fat, with their boundaries defined by the orbital retaining ligament. This distinction is vital for understanding the aging processes and planning surgical approaches. [26]
The preservation of compartments during cosmetic procedures has gained attention. Techniques focusing on repositioning rather than excising fat have been shown to yield better aesthetic outcomes by maintaining a smooth transition between the lower eyelid and cheek. [26]
The orbital fat pads contain mesenchymal stem cells that can differentiate and support tissue repair, potentially impacting conditions such as thyroid-associated orbitopathy, where increased fat and fibrosis occur in the orbit due to inflammation and immune activity. [27]
Conjunctiva
The conjunctiva is a smooth, translucent mucous membrane. Palpebral conjunctiva lines the posterior surface of the lids as tarsal conjunctiva (from the mucocutaneous junction of the lid margin to the tarsal plate border) and continues as orbital palpebral conjunctiva into the fornix. Tarsal conjunctiva is adherent to the tarsus, while a submucosal lamina propria underlies orbital palpebral conjunctiva and allows dissection from the vascular Müller muscle. At the depths of the fornices, the conjunctiva reflects anteriorly onto the globe as bulbar conjunctiva.
The blood supply for the palpebral conjunctiva comes from the vascular arcades of the eyelids. Venous drainage occurs from the small vessels of the eyelid to the conjunctival veins. These veins further drain into the orbital and facial veins. The tarsal and orbital conjunctiva has a rich vascular network. The dense capillary network in the subepithelial lamina helps meet the metabolic demands of the cornea during sleep. The blood supply to the bulbar conjunctiva is through the palpebral arcades and the anterior ciliary arteries. Lymphatic drainage occurs into the preauricular and submandibular lymph nodes. [1]
The conjunctival epithelium consists of stratified squamous and columnar cells, interspersed with goblet cells responsible for secreting mucins, which are vital for tear film stability. The thickness of the conjunctival epithelium varies, typically ranging from 3 to 5 cell layers, with a higher concentration of goblet cells located near the fornices. [28] Research suggests that goblet cells predominantly express MUC5AC, a gel-forming mucin critical for maintaining ocular surface moisture. [28, 29]
Studies focused on conjunctival stem cells showed presence of basal epithelial layer especially higher concentrations in specific areas such as the medial canthal region. This is significant for understanding epithelial renewal mechanisms and developing therapies for conjunctival disorders. [29]
Research has also documented changes in conjunctival thickness associated with age, noting that younger individuals tend to have a thicker conjunctival tissue. This finding is important for understanding age-related ocular conditions. [30]
The conjunctiva serves not only as a barrier but also as an active participant in immune defense. It contains conjunctiva-associated lymphoid tissue (CALT), which plays a role in local immune responses. The presence of various immune cells within its structure helps protect against pathogens that may enter through the ocular surface. [31]
Nerves
Sensory innervation of the eyelids is subserved by terminal branches of the ophthalmic (cranial nerve [CN] V1) and maxillary (CN V2) divisions of the trigeminal nerve (CN V). Within the superior orbit, the frontal branch of the ophthalmic division of the trigeminal nerve travels anteriorly between the periorbita of the roof and the levator muscle. Midway along the roof, it divides into a larger supraorbital nerve and a smaller supratrochlear nerve. Terminal branches of these nerves supply sensation to the upper eyelid and forehead.
The supraorbital nerve exits the orbit through the supraorbital notch or supraorbital foramen. It subserves sensation to the upper eyelid and forehead skin, except for a midline vertical strip, which is supplied by the supratrochlear nerve. The supratrochlear nerve exits the orbit just lateral to the bony origin of the corrugator supercilii muscle, enters this muscle, and divides into its terminal sensory branches.
The infratrochlear nerve, a terminal branch of the nasociliary nerve (CN V1), supplies the skin and conjunctiva of the medial canthus, the most medial aspect of the eyelids, and the nasolacrimal sac. The sensory supply of the remaining lower eyelid is provided by the infraorbital nerve (CN V2) and the zygomaticofacial nerve (CN V2). The zygomaticofacial nerve supplies skin to the lateral lower eyelid, while the palpebral branch of the infraorbital nerve supplies the central lower eyelid skin and conjunctiva.
Branches of the facial nerve innervate the muscles of facial expression. The frontal and zygomatic branches of CN VII innervate the orbicularis oculi muscle; the frontal branch of CN VII innervates the forehead muscles.
The orbicularis oculi is innervated by multiple motor branches from the branches of CN VII; in the lower eyelid, they enter the inferior edge of the orbicularis oculi, with branches lateral and medial to the lateral limbus, and there is no single dominant branch for the supply. Thus, in resection of the orbicularis oculi in lower lid surgery, preserving the pretarsal portion alone may not sufficiently support the lower lid. Conversely, if one single branch is injured, the adjacent branches can reinnervate the muscle by sprouting. [32]
The LPS is innervated by the superior branch of the oculomotor nerve, entering the muscle from its inferior surface in its posterior third. Müller's muscle (and the inferior tarsal muscle) requires sympathetic innervation. Postganglionic sympathetic fibers arise from the superior cervical ganglion and travel superiorly in the neck as a plexus with the internal carotid artery. The fibers take an intracranial course to the cavernous sinus, where they travel through the superior orbital fissure into the orbit via the CN branches.
Within the orbit, the exact pathways for sympathetic innervation of the superior and inferior tarsal muscles are unknown, but some evidence suggests that sympathetic fibers travel with the extraocular muscle motor nerves before termination on the target muscles.
Vessels and Lymphatics
The arterial supply of the eyelids is primarily derived from contributions of both the internal and external carotid arteries. [1]
The internal and external carotid arteries contribute to lid arterial supply. The internal carotid arterial supply is from the terminal branches of the ophthalmic artery medially (giving supraorbital, supratrochlear, and dorsal nasal branches) and the lacrimal artery laterally.
In the medial upper eyelid, two medial palpebral arteries arise from the ophthalmic artery as the superior and inferior marginal vessels and pass laterally — one to supply the upper lid and one to supply the lower lid. The inferior marginal vessel is a branch of the superior marginal vessel and passes deep to the MCT and canaliculi for about 10 mm before passing into the lower eyelid proper. These marginal vessels pass horizontally as marginal arcades.
The marginal arcades lie on the anterior tarsal surface approximately 4 mm and 2 mm from the upper and lower eyelid margin, respectively. In the upper lid, a peripheral arcade arises from the marginal arcade and lies on the anterior surface of the Müller muscle, just above the superior tarsal border, where it is susceptible to injury during blepharoptosis surgery. In the lower lid, no (or only a rudimentary) peripheral arcade exists.
Laterally, the lacrimal artery pierces the orbital septum to give two lateral palpebral arteries. They pass medially, one to the upper eyelid and the other to the lower eyelid, and anastomose with the marginal arcades.
The external carotid artery contributes via branches of the facial artery, the superficial temporal artery, and the infraorbital artery. The facial artery provides the angular artery, which passes to the medial canthal region, anastomosing with the dorsal nasal artery. The superficial temporal artery supplies eyelid anastomoses via the transverse facial and zygomatic branches. The infraorbital artery exits the infraorbital foramen as a terminal branch of the maxillary artery, anastomosing with vessels of the lower eyelid.
Lymphatic drainage
The eyelids and conjunctiva have a rich lymphatic drainage. Most of the upper lid and the lateral half of the lower lid drain into the preauricular lymph nodes. The medial portion of the upper lid and the medial half of the lower lid drain into the submandibular nodes by way of vessels that follow the angular and facial vessels.
Both superficial and deep lymphatic systems interconnect in these areas. The superficial collectors travel through subcutaneous fat, while deep collectors run beneath the orbicularis oculi muscle, eventually reaching the preauricular nodes. [33]
Research has highlighted the importance of these lymphatic pathways not just in normal physiology but also in pathologic conditions. Active lymphatic drainage has aqueous humor that can drain from the eye to cervical lymph nodes. This process is vital for maintaining intraocular pressure and can have therapeutic implications for conditions such as glaucoma. [34]
Studies have shown that the presence of lymphatic vessels in ocular tissues is not uniform; while the conjunctiva is rich in lymphatics, other structures such as the cornea typically lack them unless induced by inflammatory processes. This heterogeneity suggests that the conjunctiva plays a critical role in ocular immunity and inflammation resolution. [35]
The lymphatic system in the eye also serves as a conduit for immune responses. Findings indicate that there is a shared immune circuit between the posterior eye and central nervous system (CNS), allowing for coordinated immune responses. This connection has the potential for new therapeutic strategies targeting both ocular and CNS diseases. [36]
-
Orbicularis oculi muscle anatomy. (A) Frontalis, (B) corrugator superciliaris, (C) procerus, (D) orbital orbicularis, (E) preseptal orbicularis, (F) pretarsal orbicularis.
-
Upper eyelid anatomy.
-
Lower eyelid anatomy.
-
Medial canthus.
-
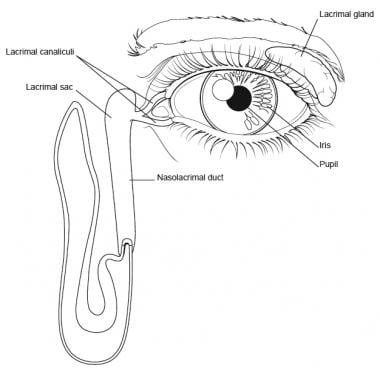
Eye and lacrimal duct.