Background
A pleural effusion is collection of fluid abnormally present in the pleural space, usually resulting from excess fluid production and/or decreased lymphatic absorption. [1] (See the images below.) It is the most common manifestation of pleural disease, and its causes occupy a spectrum ranging from cardiopulmonary disorders with systemic inflammatory conditions to malignancy.
Pleural effusions are also commonly noted in patients diagnosed with pneumonia (14-44% of patietns admitted for pneumonia), and 40% of these cases may be complicated by parapneumonic effusion or abscess. These may be categorized as uncomplicated, complicated, or empyema thoracis. Management varies, depending on the clinical presentation and the imaging findings, but it often involves drainage with diagnostic, therapeutic, or combined intent. A combined approach that includes antibiotics, intrapleural enzymatic therapy, or surgical intervention is often necessary to achieve improved outcomes.
Of the approximately 1.5 million pleural effusions diagnosed in the United States each year, more than 150,000 are due to new cases of malignant pleural effusion (MPE). Approximately 15% of cancer patients eventually develop MPEs. [2] MPEs are diagnosed on the basis of the presence of tumor cells in pleural fluid cytology or pleural tissue biopsy. They usually signify incurable disease with considerable morbidity and a dismal mean survival (< 1 y). [3]
It is important to differentiate MPEs from paramalignant pleural effusions, which have a different pathophysiology and a different prognosis. Paramalignant effusions are associated with active malignancy, but without any cytologic or pathologic evidence of malignant involvement of the pleural space. These effusions may result from bronchial obstruction, pulmonary embolism, or postobstructive atelectasis with transudative effusion, or they may occur as side effects of cancer treatment. [3]
Heart failure is another common cause of pleural effusion. Such effusions are often bilateral in presentation and are frequently associated with other signs of heart failure, such as bilateral leg swelling. Pulmonary edema and respiratory failure may be noted. Medical management is often the primary modality, with diuretics administered to lower fluid volume and, potentially, vasodilators (eg, nitroglycerin) to reduce afterload. These effusions are likely to recur, with drainage maneuvers serving only as temporizing measures.
Anatomy
In a healthy individual, the pleural space (cavity) is a potential space sandwiched between the parietal and visceral pleurae. The parietal pleura completely lines the inner chest-wall surface of the thoracic cavity, including the bilateral medial mediastinum, the subcostal left and right diaphragmatic leaflets, and the innermost muscle surface of the ribs and associated musculature. The visceral pleura tightly and completely envelops both lungs, folding into the interlobar fissures and meeting the parietal pleura at the hilar root of the lungs. The right and left pleural cavities are separated by the anterior and posterior mediastinum.
In healthy patients, the potential space of the pleural cavity plays a vital role in respiration, joining the natural outward movement of the chest wall to the natural inward movement of the lungs via the following two mechanisms:
-
First, the potential space's relative vacuum sustains the visceral and parietal pleurae's extreme adherence and is uninterrupted and not disrupted
-
Second, a diminutive volume of pleural fluid (normally calculated at 0.1-0.2 mL/kg of body weight) serves as a lubricant to facilitate the normal physiologic sliding motion of the two pleural surfaces against each other during inspiration and expiration [4]
This small volume of lubricating pleural fluid, containing a small amount of protein (< 1.5 g/dL), is maintained via a delicate balance between hydrostatic and oncotic pressure. Fluid inflow is from the capillaries lining the parietal pleura, and absorption is facilitated by the visceral capillaries (~90%) and the lymphatic vessels (~10%). Disturbances in any of these mechanisms in the secretion or drainage of pleural fluid can manifest as a pleural effusion. [5, 6]
Pathophysiology
The normal pleural space contains approximately 10 mL of fluid, representing the balance between (1) hydrostatic and oncotic forces in the visceral and parietal pleural capillaries and (2) persistent sulcal lymphatic drainage. Pleural effusions may result from disruption of this natural balance.
A pleural effusion is rarely a primary disorder; more commonly, it heralds an underlying disease process that may be pulmonary or nonpulmonary in origin and, furthermore, may be acute or chronic. [7, 8] Although the etiologic spectrum of pleural effusion can be extensive, most pleural effusions are caused by congestive heart failure (CHF), pneumonia, malignancy, or pulmonary embolism (PE).
The following mechanisms may play a role in the formation of pleural effusion:
-
Altered permeability of the pleural membranes (eg, inflammation, malignancy, PE)
-
Reduction in intravascular oncotic pressure (eg, hypoalbuminemia due to nephrotic syndrome or cirrhosis)
-
Increased capillary permeability or vascular disruption (eg, trauma, malignancy, inflammation, infection, pulmonary infarction, drug hypersensitivity, uremia, pancreatitis)
-
Increased capillary hydrostatic pressure in the systemic or pulmonary circulation (eg, CHF, superior vena cava syndrome (SVCS)
-
Reduction of pressure in the pleural space (eg, from inability of the lung to fully expand during inspiration); this is known as "trapped lung" (eg, extensive atelectasis due to an obstructed bronchus or contraction from fibrosis leading to restrictive pulmonary physiology)
-
Decreased lymphatic drainage or complete lymphatic vessel blockage, including thoracic duct obstruction or rupture (eg, malignancy, trauma)
-
Increased peritoneal fluid with microperforated extravasation across the diaphragm via lymphatics or microstructural diaphragmatic defects (eg, hepatic hydrothorax, cirrhosis, peritoneal dialysis)
-
Movement of fluid from pulmonary edema across the visceral pleura
-
Persistent increase in pleural fluid oncotic pressure from an existing pleural effusion, causing further fluid accumulation
The net results of effusion formation are flattening or inversion of the diaphragm, mechanical dissociation of the visceral and parietal pleura, and an eventual restrictive ventilatory defect as measured by pulmonary function testing. [9]
Pleural effusions are generally classified as transudates or exudates on the basis of the mechanism of fluid formation and the pleural fluid chemistry. Transudates result from an imbalance between oncotic and hydrostatic pressures, whereas exudates result from inflammatory processes of the pleura, decreased lymphatic drainage, or both. In some cases, pleural fluid may exhibit a mixture of transudative and exudative characteristics.
Etiology
Transudates
Transudates result from an imbalance in oncotic and hydrostatic pressures. Transudative effusions are usually ultrafiltrates of plasma squeezed out of the pleura as a result of these unbalanced forces in the chest. However, other mechanisms of injury may include upward movement of fluid from the peritoneal cavity or, in iatrogenic cases, direct infusion into the pleural space from misplaced (or even migrated) central venous catheters or nasogastric feeding tubes.
Causes of transudative effusions make up a relatively small and well-defined group that includes the following:
-
CHF
-
Cirrhosis (hepatic hydrothorax)
-
Atelectasis (may be due to occult malignancy or pulmonary embolism)
-
Hypoalbuminemia
-
Nephrotic syndrome
-
Peritoneal dialysis
-
Myxedema
-
Constrictive pericarditis
-
Urinothorax (usually due to obstructive uropathy)
-
Cerebrospinal fluid (CSF) leaks to the pleura (in the setting of ventriculopleural shunting or of trauma/surgery to the thoracic spine)
-
Duropleural fistula (rare, but may be a complication of spinal cord surgery)
-
Extravascular migration of central venous catheter [10]
-
Glycinothorax (rare complication of bladder irrigation with 1.5% glycine solution following urologic surgery)
Exudates
Exudative pleural effusions can result from disease in almost any organ and may be triggered by a range of mechanisms. They often require a more extensive evaluation and a more involved treatment strategy than transudative effusions do.
Mechanisms of exudative formation include the following:
-
Pleural or parenchymal inflammation
-
Impaired lymphatic drainage of the pleural space
-
Transdiaphragmatic cephalad movement of inflammatory fluid from the peritoneal space
-
Altered permeability of pleural membranes
-
Increased capillary wall permeability or vascular disruption
Pleural membranes are involved in the pathogenesis of the fluid formation. It is worth noting that the permeability of pleural capillaries to proteins is increased in disease states characterized by elevated protein content.
The more common causes of exudates include the following:
-
Malignancy (most commonly, lung or breast cancer, lymphoma, and leukemia; less commonly, ovarian carcinoma, stomach cancer, sarcomas, melanoma) [12]
-
PE
-
Collagen-vascular conditions (rheumatoid arthritis [RA], eosinophilic granulomatosis with polyangiitis, granulomatosis with polyangiitis, familial Mediterranean fever, systemic lupus erythematosus [SLE] [13, 14] )
-
Tuberculosis (TB)
-
Pancreatitis
-
Trauma
-
Postcardiac injury syndrome
-
Esophageal perforation
-
Radiation pleuritis
-
Sarcoidosis [15]
-
Fungal infection
-
Pancreatic pseudocyst
-
Intra-abdominal abscess
-
Status post coronary artery bypass graft (CABG) surgery
-
Pericardial disease
-
Meigs syndrome (benign pelvic neoplasm with associated ascites and pleural effusion) [16]
-
Ovarian hyperstimulation syndrome [17]
-
Drug-induced pleural disease (see Pneumotox.com for an extensive and searchable list of drugs that may cause pleural effusion)
-
Asbestos-related pleural disease
-
Yellow nail syndrome (yellow nails, lymphedema, pleural effusions)
-
Uremia
-
Trapped lung (localized pleural scarring with the formation of a fibrin peel prevents incomplete lung expansion, at times leading to pleural effusion)
-
Chylothorax (acute illness with elevated triglycerides in pleural fluid)
-
Pseudochylothorax (chronic condition with elevated cholesterol in pleural fluid)
-
Fistula (ventriculopleural, biliopleural, gastropleural)
-
Drowning
-
Hypothyroidism
Epidemiology
US and international statistics
Because pleural effusion is usually the manifestation of an underlying disease process, its precise incidence is difficult to determine. Nevertheless, it is the most common pleural-space disease, with an estimated annual incidence of least 1.5 million cases in the United States. [18] Most of these cases are caused by CHF, bacterial pneumonia, malignancy, and PE. Approximately 150,000 new cases of MPE are diagnosed annually. Lung and breast cancer combined account for more than 60% of MPEs, gastrointestinal (GI) and hematologic cancers account for 11% each, and other malignancies account for the remainder. [3]
In industrialized countries, the estimated prevalence of pleural effusion has been estimated at 320 cases per 100,000 people, with a distribution of etiologies related to the prevalence of underlying diseases. [7]
Age-, sex-, and race-related demographics
Pleural effusions usually occur in adults. However, they appear to be increasing in children, often in the setting of underlying pneumonia. [19] Fetal pleural effusions have also been reported and under certain circumstances may be treated before delivery. [20]
In a 2021 report from the American College of Chest Physicians (ACCP), 60% of the hospitalizations related to pleural infections were found to occur in the 18- to 64-year-old age group, and a male predominance in adult pleural infections was noted. [21] In a 2023 statement from the European Respiratory Society (ERS) and the European Society of Thoracic Surgeons (ESTS), this age group was found to account for 40% of adult pleural infections in the United Kingdom and Europe. [22] Advancing age leads to an increase in associated comorbidities, including a higher risk of pneumonia and, subsequently, pleural effusions and empyema.
Pleural effusion associated with SLE is specifically more common in women than in men. In the United States, the incidence of pleural effusion in the setting of malignant mesothelioma is higher in men, probably because of their higher occupational exposure to asbestos. Pleural effusions associated with chronic pancreatitis are more common in men, with the majority of male cases having alcohol abuse as the impetus. Rheumatoid effusions also occur more commonly in males than in females.
Given that pleural effusion is usually the manifestation of an underlying disease process, any race-related differences in frequency most likely reflect racial variations in the incidence of the causative disorder.
Prognosis
The prognosis in pleural effusion varies according to the condition’s underlying etiology. Generally, however, the complication rate is substantially lower for patients who seek medical care earlier in the course of their disease and who obtain prompt diagnosis and treatment than for patients who do not.
The morbidity and mortality of pleural effusions are directly related to the cause (and, if applicable, stage) of the underlying disease at the time of presentation, as well as to biochemical findings in the pleural fluid.
Morbidity and mortality are higher in patients with pneumonia and pleural effusions than in those in patients with pneumonia alone. Parapneumonic effusions, when recognized and treated promptly, typically resolve without significant sequelae; however, untreated or inappropriately treated parapneumonic effusions may lead to empyema, constrictive fibrosis, and sepsis.
MPEs are associated with a very poor prognosis (median survival, 4 mo; mean survival, < 1 y). [23, 24] Several studies have shown that patients with an MPE have a higher mortality than patients who have metastatic cancer without MPE. In men, the most common associated malignancy is lung cancer; in women, it is breast cancer. Median survival ranges from 3 to 12 months, depending on the malignancy. Effusions from cancers that are more responsive to chemotherapy (eg, lymphoma or breast cancer) are more likely to be associated with prolonged survival than effusions from lung cancer or mesothelioma. [25, 26]
As noted, cellular and biochemical findings in the fluid may also be indicators of prognosis. For example, a lower pleural fluid pH is often associated with a higher tumor burden and a worse prognosis. [27]
-
Large right-side pleural effusion. This effusion was noted to be malignant in nature.
-
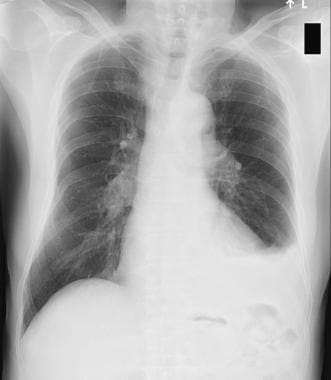
Left-side pleural effusion.
-
Left lateral decubitus film displaying freely layering left-side pleural effusion.
-
Lung entrapment with right hydropneumothorax and pleural drain in place.
-
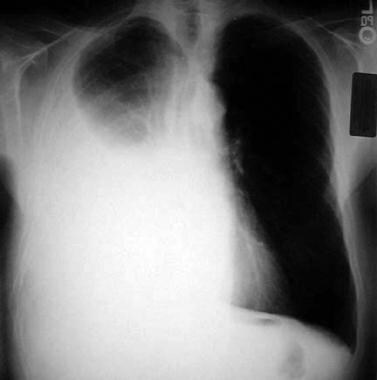
Massive right-side pleural effusion resulting in mediastinal shift to left.
-
Right-side pleural effusion after partial drainage showing improved left mediastinal shift.
-
Bilateral pleural effusions with loss of bilateral costophrenic sulci (meniscus sign). Anteroposterior upright chest radiograph. Image from Allen R Thomas, MD.
-
Isolated left-side pleural effusion with visualized loss of left lateral costophrenic sulcus. Posteroanterior upright chest radiograph. Image from Allen R Thomas, MD.
-
Ultrasonogram shows large simple effusion with anechoic fluid collection. Additionally, thoracentesis needle can be seen, showing additional utility for needle placement or preprocedural site marking.
-
Ultrasonogram of pleural space shows densely septated loculation in pleural space.
-
Ultrasonogram shows simple pleural effusion with anechoic fluid collection in subpulmonic space.
Tables
What would you like to print?
- Overview
- Presentation
- DDx
- Workup
- Treatment
- Guidelines
- Medication
- Antibiotics, Lincosamide
- Antibiotics, Other
- Anticoagulants, Hematologic
- Carbapenems
- Cephalosporins, 3rd Generation
- Cephalosporins, 4th Generation
- Diuretics, Loop
- Enzymes, Mucolytic
- Fluoroquinolones
- Glycopeptides
- Nitrates, Angina
- Nitroimidazoles
- Penicillins, Amino
- Penicillins, Extended-Spectrum
- Thrombolytics
- Show All
- Media Gallery
- References