Practice Essentials
A renal artery aneurysm (RAA) is defined as a dilated segment of renal artery with a diameter that is more than twice the diameter of a normal renal artery. [1, 2] Symptomatic RAAs can cause hypertension, pain, hematuria, and renal infarction. [3] Asymptomatic RAAs may seem benign, but the potential for rupture and fistulization increases with size. Asymptomatic patients can be referred for elective repair, but if patients are symptomatic, further investigation with possible surgical intervention should be considered.
The first published report of an RAA was in 1770 by Rouppe, who described the demise of a sailor who fell onto his right flank. Autopsy revealed a large false aneurysm with rupture. Since that time, many more case reports and case series have provided most of the data on this rare pathologic entity.
Because most RAAs are asymptomatic and are found incidentally during a workup for other intra-abdominal pathology, imaging studies are required only for preintervention planning or longitudinal follow-up care.
Indications for intervention in patients with a RAA include rupture, symptomatic RAA, RAA in a female who is pregnant or is contemplating pregnancy, diameter greater than 2 cm, enlarging RAA, and RAA associated with acute dissection. Currently, there is no consensus regarding the size at which an RAA should be repaired in an asymptomatic patient, though asymptomatic small (< 2 cm in diameter) RAAs usually are not considered to require treatment. Advances in endovascular techniques are ongoing, and this approach is preferred to open repair at many centers. [4]
Anatomy
The renal arteries arise from the aorta at the level of the intervertebral disk between L1 and L2. Cadaveric studies have shown that more than one renal artery is present in 15% of cases on the right side and 20% of cases on the left.
A great deal of variety can be found in the anatomy of the renal artery and its branches, but most often, the main renal artery splits into an anterior and a posterior division. Within the hilum, the anterior division gives rise to apical, anterior, and inferior segmental branches. Segmental vessels then penetrate the renal parenchyma to become lobar, interlobar, arcuate, or interlobular arteries or afferent arterioles, then finally reach the capillaries and glomeruli. [5]
Measurements of renal artery diameter can differ, depending on the imaging modality used. In one study, ultrasonography (US) reported mean renal artery measurements of 5.04 ± 0.74 mm; with angiography, they were found to be 5.68 ± 1.19 mm. In this study, the authors also determined that when accessory renal arteries were identified, the main renal artery measurements were significantly smaller in diameter than when one renal artery was present. [6]
RAAs can be classified in relation to the parenchyma of the kidney (see the image below). Extraparenchymal aneurysms predominate, comprising approximately 85% of all RAAs [7, 8] ; the other 15% are intraparenchymal. Of the extraparenchymal type, roughly 70% are saccular, 20% are fusiform, and 10% are dissecting. [9]
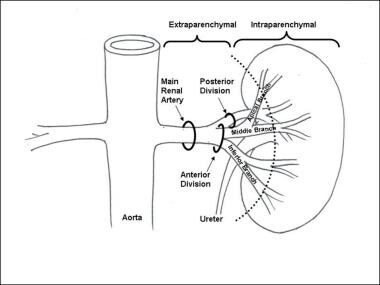 Schematic of renal artery anatomy. The aneurysm location can be classified as extraparenchymal or intraparenchymal.
Schematic of renal artery anatomy. The aneurysm location can be classified as extraparenchymal or intraparenchymal.
Of patients with RAAs, 20% present with bilateral pathology, and 30% have multiple aneurysms. [8] RAAs occur with equal frequency in men and women, though ruptures are more common in reproductive-age women.
Pathophysiology
In true aneurysms, a weakening then dilatation of all layers of the arterial wall occurs. In fibromuscular dysplasia (FMD), the degenerative fibroplasia-type changes lead to this wall weakening. Often, renal artery stenosis is associated. [10, 8] Most patients with FMD are healthy, young, hypertensive women, and on angiography the renal artery appears as a string of beads, with the aneurysm at the renal artery bifurcation.
Ehlers-Danlos syndrome is an autosomal dominant disorder characterized by fragility of medium-sized and large arteries due to type III procollagen deficiency. This condition leads to dissections and aneurysms in any artery, including the renal arteries. [11]
In false aneurysms, or pseudoaneurysms, there is a focal disruption in one or every layer of the artery that causes a saccular outpouching at the weaken area. In blunt trauma, anterior displacement of the relatively mobile kidneys with rapid deceleration generates tension in the vascular pedicle that causes a fracture of the intima, predisposing it to subintimal dissection and then aneurysmal degeneration. Another mechanism involves direct arterial-wall contusion against the vertebral bodies.
Anastomotic leaks from previous renal artery reconstructive procedures become walled off by the body, creating a pseudoaneurysm. In this situation, the wall of the aneurysm contains only fibrotic/inflammatory tissue. Iatrogenic endovascular-related aneurysms are caused by intimal trauma and focal dissection, leading to aneurysmal degeneration. Spontaneous renal artery dissections cause aneurysms by the same mechanism described above. [2]
Intraparenchymal aneurysms are believed to arise primarily from inflammatory changes of the vessel wall. These commonly develop into microaneurysms. Intrarenal aneurysms are usually found in multiples and are often associated with arteriovenous fistulas.
Although pregnancy is not associated with an increased incidence of RAA formation, it is associated with a higher rate of rupture. The increased blood flow, intra-abdominal pressure, and vessel-wall changes due to the hormonal and metabolic changes associated with gestation are believed to be contributory. Most ruptures occur late in the pregnancy (usually in the third trimester) and are left renal artery–predominant. [12]
In the pediatric age group, RAAs are due to trauma, infection, arteritides, Kawasaki disease, or vascular dysplasias. Multiple idiopathic arterial aneurysms that include renal artery involvement have been described but are extremely rare. [13]
Etiology
Many causes of RAA exist, each with different morphologies and locations along the renal artery. The lesions can be grouped into three main categories as follows.
True aneurysms include all layers of the artery and are usually inherited disorders. They can be fusiform or saccular (75% of all true RAAs) in appearance and are extraparenchymal in 90% of cases. [7] Causes include the following:
-
FMD
False aneurysms (pseudoaneurysms) do not include all layers of the artery, are usually acquired, are saccular in appearance, and can be extraparenchymal or intraparenchymal. Causes include the following:
-
Blunt abdominal trauma
-
Anastomotic
-
Iatrogenic during endovascular procedures
-
Spontaneous [15]
-
Dissection
-
Mycotic [16]
-
Kawasaki disease [17]
Intrarenal aneurysms are either true or false aneurysms within the renal parenchyma and account for fewer than 10% of all RAAs. They deserve special classification because their management is usually with nephrectomy or coil embolization. Causes include the following:
-
Polyarteritis nodosa
-
Tuberculosis
-
Neurofibromatosis
Epidemiology
Autopsy studies indicate that the incidence of RAA is in the range of 0.01-0.09%. [18] In selected patients who undergo renal arteriography, a higher incidence, 0.3-1%, has been reported. [19] In another study using computed tomography (CT) angiography (CTA), the incidence was 0.7%. [20] In one of the largest series over a 16-year period, 62 patients had RAA repair. The average age was 46 ± 18 years, and 68% were women. [21]
Overall, the average age for patients to present with RAAs is between the ages of 40 and 60 years, with a female predominance owing to the increased prevalence among patients with FMD.
Prognosis
The morbidity and mortality associated with elective RAA repair are very low. Many authors have reported no mortality and minimal morbidity after surgery. [22, 23, 8, 24] Surgical repair of RAA appears to have long-term durability, though most reported series have been small and from single centers.
In a study that included 2709 patients undergoing open or endovascular elective repair of isolated RAAs between 2000 and 2011, Buck et al found no significant differences in mortality and overall complication rate between the two types of repair. [25]
In a systematic review and meta-analysis (38 studies) assessing the outcomes of endovascular exclusion (EVR; n = 1540), open repair (OR; n = 2377), and ex-vivo repair with renal autotransplantation (ERAT; n = 109) in the treatment of RAAs, Choksi et al found the outcomes of EVR and OR to be comparable, with EVR being associated with a shorter length of stay. [26] ERAT, currently performed for distal RAAs, carried a higher risk of infarction and nephrectomy.
The prognosis after rupture of an RAA has improved in the past few decades. One review found that mortality dropped from 62% before 1949 to 6% after 1970. Rupture of RAA during pregnancy still carries a high mortality. According to one report, renal artery rupture and its treatment resulted in death of the mother in 56% of the cases and death of the fetus in 78% of the cases. [12]
The cure rate of hypertension may be as high as 50-100% in selected patients with RAAs associated with renal artery stenosis. [22, 27, 23]
-
Schematic of renal artery anatomy. The aneurysm location can be classified as extraparenchymal or intraparenchymal.
-
(A) Aortogram with calcified left renal artery aneurysm (RAA). (B-C) Same RAA in magnified view, demonstrating the RAA is saccular, arising from the main renal artery.
-
(A) Computed tomography scan and (B) arteriogram of the same patient with a saccular left renal artery aneurysm at a segmental renal artery branch.
-
Magnetic resonance imaging of a patient with 2 left renal artery aneurysms. Both are saccular, one is at a segmental branch (closed arrow) and the other is intrarenal (open arrow). Of note: this patient also has a congenital absence of the right kidney.
-
(A) Extraparenchymal saccular aneurysm. (B) Tangential excision with patch angioplasty.
-
(A) Fibromuscular dysplasia with string-of-beads appearance and wide-necked extraparenchymal saccular aneurysm. (B) Aneurysm excision with reconstruction using a bypass graft.
-
Arteriogram of saccular renal artery aneurysm after coil embolization.
-
Subsequent expansion of aneurysm 6 months after coil embolization.
-
(A) Renal artery stenosis with poststenotic fusiform aneurysm. (B) Exclusion of aneurysm and dilatation of stenosis with endovascular stent graft.

