Practice Essentials
Diabetic foot ulcers, as shown in the images below, occur as a result of various factors, such as mechanical changes in conformation of the bony architecture of the foot, peripheral neuropathy, and atherosclerotic peripheral arterial disease, all of which occur with higher frequency and intensity in persons with diabetes. [1, 2]
Nonenzymatic glycation predisposes ligaments to stiffness, while neuropathy causes loss of protective sensation and loss of coordination of muscle groups in the foot and leg, with the latter two increasing mechanical stresses during ambulation.
Of the more than 500 million people worldwide who are estimated to have diabetes, the risk of developing foot ulcers in their lifetime is 19-34%, with 10% dying within 1 year of their first diagnosis of diabetic foot ulcer. A lower-extremity amputation will be necessary in about 20% of persons with a diabetic foot ulcer. [3]
Physical examination of the extremity that has a diabetic ulcer can be divided into examination of the ulcer, examination of the feet, assessment for the possibility of vascular insufficiency, [4] and assessment for the possibility of peripheral neuropathy.
Diabetic foot ulcers can be staged using the Wound, Ischemia, and foot Infection (WIfI) threatened limb classification system. This system allows communication between providers and provides risk stratification for major amputation. [5] Blood work should be obtained, such as a complete blood count (CBC), a comprehensive metabolic panel, and hemoglobin A1c (HbA1c), as well as inflammatory markers when infection is suspected. Weight-bearing radiographs of the affected limb should be obtained.
The management of diabetic foot ulcers requires offloading the wound, [6, 7] daily saline or similar dressings to provide a moist wound environment, [8] débridement when necessary, antibiotic administration with or without surgical intervention if osteomyelitis or soft tissue infection is present, [9, 10] optimal control of blood glucose, and evaluation and correction of peripheral arterial insufficiency. [11]
All patients harboring diabetic foot ulcers should be evaluated by qualified surgical specialists, who will consider débridement, reconstructive surgery on bony architecture, vascular reconstruction, and options for soft tissue coverage.
It is prudent to address the underlying etiologies in diabetic foot ulcers for wound care modalities to be successful. Without addressing the osseous deformities and muscular imbalances as well as infections and vascular insufficiency, there will be minimal benefit in employing advanced wound care dressings.
For more information, see Type 1 Diabetes Mellitus and Type 2 Diabetes Mellitus.
Pathophysiology
Atherosclerosis and peripheral neuropathy occur with increased frequency in persons with diabetes mellitus (DM).
Trophic changes
Non-enzymatic glycosylation of skin and connective tissue, along with decreased collagen production, in people with diabetes result in alterations in the biomechanics in the diabetic foot. This is frequently seen in the Achilles tendon, where increased stiffness results in a contracture that limits ankle dorsiflexion, a condition known as equinus. Equinus has been associated with diabetic foot ulcers, as it increases plantar pressures in the forefoot and midfoot.
Diabetes-related atherosclerosis
Overall, people with diabetes mellitus (DM) have a higher incidence of atherosclerosis, thickening of capillary basement membranes, arteriolar hyalinosis, and endothelial proliferation. Calcification and thickening of the arterial media (Mönckeberg sclerosis) are also noted with higher frequency in persons with diabetes, although whether these factors have any impact on the circulatory status is unclear.
People with diabetes, like individuals who are not diabetic, may develop atherosclerotic disease of large-sized and medium-sized arteries, such as aortoiliac and femoropopliteal atherosclerosis. However, significant atherosclerotic disease of the infrapopliteal segments is particularly common in the population with diabetes. Underlying digital artery disease, when compounded by an infected ulcer in close proximity, may result in complete loss of digital collaterals and precipitate gangrene.
The prevalence of this form of arterial disease in persons with diabetes is thought to result from a number of metabolic abnormalities, including high low-density–lipoprotein (LDL) and very-low-density–lipoprotein (VLDL) levels, elevated plasma von Willebrand factor, inhibition of prostacyclin synthesis, elevated plasma fibrinogen levels, and increased platelet adhesiveness.
Diabetic peripheral neuropathy
The pathophysiology of diabetic peripheral neuropathy is multifactorial and is thought to result from vascular disease occluding the vasa nervorum; endothelial dysfunction; deficiency of myoinositol-altering myelin synthesis and diminishing sodium-potassium adenine triphosphatase (ATPase) activity; chronic hyperosmolarity, causing edema of nerve trunks; and the effects of increased sorbitol and fructose. [12]
Motor dysfunction of peripheral nerves in diabetic neuropathy leads to muscular imbalances in the diabetic foot. Muscle wasting of the intrinsic pedal muscles leads to overpowering of the spared extrinsic muscles, which results in significant forefoot deformities such as claw toes or hammer toes. [13, 14] Autonomic dysfunction of the peripheral nervous system may lead to sudomotor dysfunction. This will result in dry, cracked skin, which is more prone to injury and breakdown. [15]
The loss of sensation in the foot leads to repetitive stress, unnoticed injuries and fractures, and structural foot deformities such as hammertoes, bunions, metatarsal deformities, or Charcot foot (see the image below). These issues result in further stress and eventual tissue breakdown. Additionally, unnoticed excessive heat or cold, pressure from poorly fitting shoes, or damage from a blunt or sharp object inadvertently left inside a shoe can cause blistering and ulceration. Combined with poor arterial inflow, these factors place patients with diabetes at a significantly increased risk for limb loss.
See Diabetic Neuropathy for more information.
Etiology
The etiologies of diabetic ulceration include neuropathy, [16] arterial disease, [17] pressure, [6] and foot deformity. [18] Diabetic peripheral neuropathy, present in 60% of persons with diabetes and 80% of individuals with diabetes who have foot ulcers, confers the greatest risk of foot ulceration; microvascular disease and suboptimal glycemic control contribute.
A study by Naemi et al indicated that tissue mechanics may be associated with foot ulceration in patients with diabetic neuropathy, with an evaluation of 39 patients finding that the heel pad in nonulcerated feet tended to be stiffer than in ulcerated feet. [19] These results were further elucidated in another study by Naemi and colleagues, which reported that the risk of diabetic foot ulcer is higher in patients with diabetic neuropathy who have greater plantar soft tissue thickness and lower stiffness in the area of the first metatarsal head. The investigators found that adding the mechanical properties of plantar soft tissue (stiffness and thickness) to commonly evaluated clinical parameters improved specificity, sensitivity, prediction accuracy, and prognosis strength by 3%, 14%, 5%, and 1%, respectively. [20]
The anatomy of the foot must be considered in risk calculation. A person with flatfoot (pes planus) or a high-arched foot (pes cavus) is more likely to have disproportionate stress across the foot and may have an increased risk for tissue inflammation in high-stress regions.
Charcot foot
Sensory neuropathy involving the feet may lead to unrecognized episodes of trauma. Motor neuropathy, causing intrinsic muscle weakness and splaying of the foot on weight bearing, compounds this trauma. The result is a convex foot with a rocker-bottom appearance. Multiple fractures are unnoticed until bone and joint deformities become marked. This is termed a Charcot foot (neuropathic osteoarthropathy) and most commonly is observed in diabetes mellitus, affecting about 2% of persons with diabetes.
If a Charcot foot is neglected, ulceration may occur at pressure points, particularly the medial aspect of the navicular bone and the inferior aspect of the cuboid bone. Sinus tracts progress from the ulcerations into the deeper planes of the foot and into the bone. Charcot change can also affect the ankle, causing displacement of the ankle mortise and ulceration, which can lead to the need for complex reconstruction. Failure of these complex reconstructions on poor surgical hosts leads to major limb amputations.
Epidemiology
According to a crude 2021 estimate, 38.4 million people in the United States had diabetes (11.6% of the population). [21] Of the more than 500 million people worldwide who are estimated to have diabetes, the risk of developing foot ulcers in their lifetime is 19-34%. A lower-extremity amputation will be necessary in about 20% of persons with a diabetic foot ulcer. [3]
Mortality
Mortality within 1 year of the first diagnosis of diabetic foot ulcers is 10%. [3]
Prevalence of diabetic ulcers by race
The issue of diabetic foot disease is of particular concern in the Latino communities of the Eastern United States, in African Americans, [22] and in Native Americans, with the last tending to have the highest prevalence of diabetes in the world.
See the Medscape Drugs & Diseases article Diabetic Foot Infections for more information.
Prognosis
Mortality in people with diabetes and foot ulcers is often the result of associated large vessel arteriosclerotic disease involving the coronary or renal arteries.
In assessing the health-related quality of life (HRQOL) in adults with diabetic foot ulcers, a literature review by Khunkaew et al found that such patients scored poorly on four of eight scales on the 36-Item Short Form Health Survey (SF-36), specifically, physical functioning, role physical, general health, and vitality. Risk factors for a lower HRQOL included the existence of pain, a C-reactive protein level above 10 mg/L, an ulcer size of over 5 cm2, an ankle-brachial index value of less than 0.9, a high glycosylated hemoglobin level, and a body mass index of over 25 kg/m2. [23]
Limb loss is a significant risk in patients with diabetic foot ulcers, particularly if treatment has been delayed. [24] Diabetes is the predominant etiology for nontraumatic lower extremity amputations in the United States. Half of all nontraumatic amputations are a result of diabetic foot complications, and the 5-year risk of needing a contralateral amputation is 50%. [25]
In people with diabetes who have neuropathy, [26] even if successful management results in healing of the foot ulcer, the recurrence rate is 66% and the amputation rate rises to 12%.
A study by Chammas et al indicated that ischemic heart disease is the primary cause of premature death in patients with diabetic foot ulcer, finding it to be the major source of mortality on postmortem examination in 62.5% of 243 persons with such ulcers. The study also found that in patients with diabetic foot ulcer, the mean age of death from ischemic heart disease, as derived from postmortem examination, was 5 years below that of controls. Patients with neuropathic foot ulcers were determined to have the highest risk of premature death from ischemic heart disease. [27]
A study by Chen et al indicated that following hospital treatment for diabetic foot ulcer, invasive systemic infection associated with the ulcer (DFU-ISI) is an important late complication that increases mortality risk. In the study’s patients, methicillin-resistant Staphylococcus aureus (MRSA) gave rise to 57% of the ISIs. Using Cox regression modeling, the investigators found that complicated ulcer healing and the presence of MRSA in the initial ulcer culture predicted the development of DFU-ISIs (hazard ratios of 3.812 and 2.030, respectively), with the hazard ratio for mortality risk in association with DFU-ISIs being 1.987. [28]
Patient Education
The risk of foot ulceration and limb amputation in people with diabetes is lessened by patient education stressing the importance of routine preventive foot care, daily self inspection of feet, appropriate shoes, avoidance of barefoot walking, avoidance of cigarette smoking, control of hyperlipidemia, and adequate glycemic control.
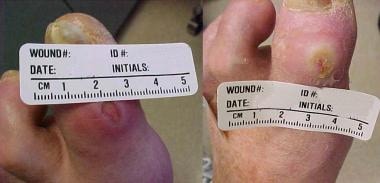
-
Diabetic ulcer of the medial aspect of left first toe before and after appropriate wound care.
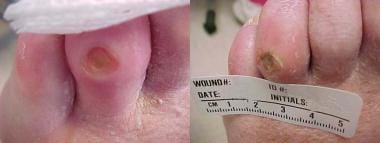
-
Diabetic ulcer of left fourth toe associated with mild cellulitis.
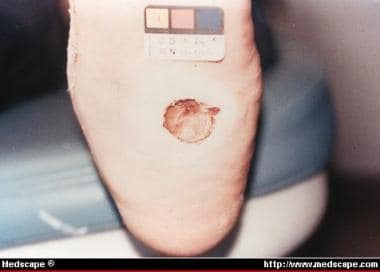
-
Charcot deformity with mal perforans ulcer of plantar midfoot.
Tables
What would you like to print?
- Overview
- Presentation
- DDx
- Workup
- Approach Considerations
- Blood Tests
- Plain Radiography
- Computed Tomography Scanning and Magnetic Resonance Imaging
- Bone Scans
- Ankle-Brachial Index
- Pulse-Volume Recording
- Ultrasonography
- Transcutaneous Tissue Oxygen Studies
- Conventional Angiography
- Alternatives to Conventional Angiography
- Staging
- Laboratory Studies
- Other Tests
- Procedures
- Show All
- Treatment
- Approach Considerations
- Management of Systemic and Local Factors
- Wound and Foot Care
- Surgical Care
- Options for Soft Tissue Coverage of the Clean but Nonhealing Wound
- Hyperbaric Oxygen Treatment
- Dietary Changes
- Restriction of Activity
- Measures for Prevention of Diabetic Ulcers
- Consultations
- Long-Term Monitoring
- Show All
- Guidelines
- Medication
- Media Gallery
- Tables
- References