Background
Toxic epidermal necrolysis (TEN) is a potentially life-threatening dermatologic disorder characterized by widespread erythema, necrosis, and bullous detachment of the epidermis and mucous membranes, resulting in exfoliation and possible sepsis and/or death. [1, 2, 3] Mucous membrane involvement can result in gastrointestinal hemorrhage, respiratory failure, ocular abnormalities, and genitourinary complications.
TEN is most commonly drug induced. [1, 2, 4, 3] However, the disorder occasionally has other potential etiologies, including infection including COVID-19, [5, 6] malignancy, and vaccinations, including following COVID-19 vaccination. [7] TEN is idiosyncratic, and its occurrence is not easily predicted.
Some authors believe that Stevens-Johnson syndrome (SJS; also known as erythema multiforme major) is a manifestation of the same process involved in TEN, with the latter involving more extensive necrotic epidermal detachment. TEN involves more than 30% of the body surface, whereas SJS involves less than 10%.
A classification system, based largely on the extent of epidermal detachment and morphology of the skin lesions, aids in differentiating opposite spectrums of the same disease entity. [8] This system comprises the following:
-
TEN with spots
-
TEN without spots
-
Overlap Stevens-Johnson syndrome and TEN (SJS-TEN)
TEN with spots is defined as widespread, irregularly shaped erythematous or purpuric macules with blistering that occurs on all or part of the macule. Blisters become more confluent and result in detachment of the
Pathophysiology
The pathophysiology of TEN has not been fully elucidated; however, various theories have received wide acceptance. TEN is believed to be an immune-related cytotoxic reaction aimed at destroying keratinocytes that express a foreign antigen. [1, 2, 3]
TEN mimics a hypersensitivity reaction, with its characteristic delayed reaction to an initial exposure and an increasingly rapid reaction with repeated exposure.
The widespread epidermolysis and blistering of TEN results from keratinocyte apoptosis—an organized series of biochemical reactions leading to cell changes and cell death. [14] However, the number of inflammatory T cells in the skin of patients with TEN is variable and perhaps too low to explain the widespread destruction. [15]
There is evidence supporting several immunopathologic pathways leading to keratinocyte apoptosis in TEN, including the following:
-
Fas ligand activation on keratinocyte membranes leading to death receptor–mediated apoptosis [16]
-
Release of destructive proteins (perforin and granzyme B) from cytotoxic T lymphocytes (CTLs) generated from an interaction with cells expressing major histocompatability complex (MHC) class I [17]
-
Drug-induced secretion of granulysin from CTLs, natural killer cells, and natural killer T cells [20]
Precisely how the inciting agent triggers the proposed pathways is yet to be elucidated.
Etiology
TEN can be induced by drugs or infection or can be idiopathic. [21, 1, 2, 3] Medications are the major precipitating cause. Numerous medications have been implicated, [22] including antibiotics, antiepileptic drugs, nonsteroidal anti-inflammatory drugs (NSAIDs), ampicillin, allopurinol, corticosteroids (topical and systemic), and the antiretroviral drugs nevirapine and abacavir. [23, 24] TEN usually occurs during the first course of therapy with a drug (ie, without sensitization).
Antibacterial drugs associated with TEN include the following:
-
Sulfonamides (4.5 cases per million users per week)
-
Chloramphenicol
-
Macrolides (eg, azithromycin, clarithromycin, erythromycin, telithromycin) [25]
-
Penicillins
Anticonvulsants associated with TEN include the following:
-
Phenobarbital
-
Phenytoin [28]
-
Carbamazepine
-
Valproic acid
-
Lamotrigine
TEN in patients taking anticonvulsants has most often been reported within 2 months of starting the drug. However, some cases associated with long-term use have been reported.
NSAIDs associated with TEN include the following:
-
Phenylbutazone and oxybutazone - Implicated most commonly, although they are no longer available in the United States
-
Oxicams (eg, piroxicam, tenoxicam) - Implicated more often than other NSAIDs
-
Ibuprofen
-
Indomethacin
-
Sulindac
-
Tolmetin
With allopurinol, risk is not constant over time. Patients have a 5.5 relative risk. However, during the first 2 months of therapy, the relative risk is 52, and the long-term therapy risk is 0.5.
No laboratory test is able to confirm a specific drug etiology. A causal link is suggested when TEN occurs during the first 4 weeks of medication therapy, usually between 1 and 3 weeks. Drugs with longer half-lives and those with circulating active metabolites may result in more fulminant disease.
Infectious agents (ie, Mycoplasma pneumoniae, herpes virus, hepatitis A), immunizations (eg, meningococcal vaccine), and bone marrow or solid organ transplantation have also been associated with TEN. [29]
Epidemiology
In the United States, the annual frequency of TEN is reported to be 0.22-1.23 cases per 100,000 population. In the HIV-positive population, the incidence of TEN increases to 1 case per thousand per year. [30]
Worldwide, the average annual incidence of TEN is 0.4-1.3 cases per million population. [31] In 1992, the cumulative incidence of TEN and SJS in Germany was 1.9 cases per million population. A French survey of dermatologists and health care facilities reported an annual incidence of 1 case per million population.
Race-, sex-, and age-related demographics
A genetic predilection toward carbamazepine-induced TEN has been observed in HLA-B*1502–positive patients in mainland southeast Asian people from China to India. The US Food and Drug Administration recommends screening for the HLA-B*1502 allele before initiating carbamazepine in patients of Asian ancestry. [32] The HLA-B*58:01 allele is associated with allopurinol-induced TEN in Han Chinese people. HLA-A*66:01, HLA-B*44:03, and HLA-C*12:03 have been associated with cold medicine-TEN with severe ocular complications in patients who had taken cold medicines in the 1-14 days prior to onset of the disease. The HLA-B*44:03 (odds ratio, 5.50) and HLA-C*12:03 (OR, 8.79) alleles were associated with a less-robust tisk of cold medicine-TEN only in European patients. [33]
Registration databases from Tawain, Thailand, Japan, Malaysia, Singapore, Hong Kong, the Philippines, and mainland China (Fujian) identified that from 1998-2017, greater than 50% of cases of SJS/TENS involved carbamazepine, allopurinol, phenytoin, lamotrigine, and sulfamethoxazole. Oxacarbazepine, sulfasalazine, COX-II inhibitors, and strontium ranelate (not approved by the Food and Drug Administration but used in more than 70 countries as a treatment option for postmenopausal osteoporosis) have been identified as potential new causes of SJS/TENS in Asian patients. Other medications known to cause SJS/TENS such as oseltamavir, terbinafine, and sorafenib, were not associated with any cases in Asian patients enrolled in these databases. [34]
For unclear reasons, TEN appears to have a predilection for females. The female-to-male ratio is 1.5:1. [35]
TEN may occur in all age groups; however, the mean age of patients with TEN is reported to be between 46 and 63 years. Infection is more commonly implicated as an etiology in children, whereas medication exposure is more common in adults. Elderly persons may be at greater risk because of their tendency to use multiple medications.
Prognosis
The estimated mortality associated with TEN varies widely in different reports, from 10-70%. Outcome depends in part on the quality of care and the rapidity with which treatment is initiated. [2]
The re-epitheliazation period lasts between 1 and 3 weeks, depending on the extent and severity of the clinical picture. [36]
Septicemia and multisystem organ failure are the primary causes of death. Epithelial loss results in vulnerability to bacterial and fungal infections. Sloughing of stratified epithelium of mucosal membranes can result in GI hemorrhage, respiratory failure, ocular abnormalities, and genitourinary lesions. Significant fluid loss from extensive skin exfoliation and an inability to tolerate oral intake can lead to hypovolemia, acute tubular necrosis, and shock.
Age, extent of epidermal involvement, and serum urea level are said to be the most important prognostic factors in TEN. [37] Mortality rates in children are much lower than in adults. [38] Elderly patients have a poor prognosis.
Other negative prognostic factors include the following:
-
Elevated blood urea nitrogen (BUN) and serum creatinine levels
-
Respiratory failure
-
Multiple drugs
-
Thrombocytopenia
-
Lymphopenia
-
Neutropenia
-
Leukopenia
-
Sepsis
Severity-of-illness score
A severity-of-illness score that estimates the risk of death in TEN (SCORTEN) has been developed and validated. [39] Each of the following independent prognostic factors is given a score of 1:
-
Age >40 years
-
Heart rate >120 beats per minute
-
Cancer or hematologic malignancy
-
Involved body surface area >10%
-
Blood urea nitrogen level >10 mmol/L (28 mg/dL)
-
Serum bicarbonate level < 20 mmol/L (20 mEq/L)
-
Blood glucose level >14 mmol/L (252 mg/dL)
The number of positive criteria and the corresponding mortality rates are as follows:
-
0: 1 to 3%
-
2: 12%
-
3: 35%
-
4: 58%
-
5 or more: 90%
Sequelae
Major sequelae are generally limited to the affected organ systems (ie, the skin and mucosal membranes).
Cutaneous sequelae of TEN include the following:
-
Changes in skin pigment (hypopigmentation or hyperpigmentation; sun exposure must be avoided for several months because ultraviolet light can worsen hyperpigmentation; sunblock is recommended)
-
Nail loss and nail dystrophy
-
Hypohidrosis (inability to sweat)
-
Scarring, alopecia, and hypertrophic scarring
-
Dermal desiccation, causing deep dermal wounds
-
Chronic xerostomia
-
Esophageal strictures
-
Vulvovaginal synechiae
-
Phimosis [40]
-
Chronic erosion of the mouth and genitalia
Ocular complications generally result from abnormal keratinization of the tarsal conjunctiva. A Sjogrenlike syndrome with decreased lacrimal secretion causes dry eye and predisposes to corneal abrasions and corneal scarring with neovascularization. In addition, patients have been reported to have palpebral synechiae, entropion, or symblepharon (adhesion of the eyelids). [41, 42]
A study by Power and colleagues found that 50% of patients with TEN developed ocular complications. [43] Patients treated with steroids fared no better than those treated without steroids. Therefore, TEN remains a common cause of visual loss in a significant number of patients. Ultimately, 5-9% of patients can become blind as a result of some of these complications.
Up to 28% of women with vaginal involvement in the acute phase suffered from long-term sequelae, including burning sensation, dyspareunia, and postcoital bleeding from adhesions and stenosis. Male genitalia synechiae may require circumcision. [44]
-
Toxic epidermal necrolysis (TEN) ulcer in great toe (initial infection).
-
Hemorrhagic crusting of mucous membranes in toxic epidermal necrolysis (TEN).
-
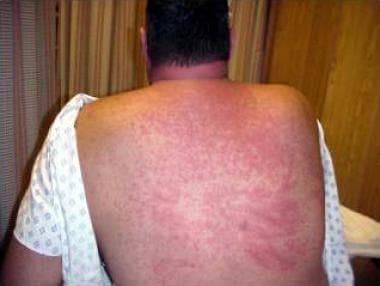
Maculopapular rash in toxic epidermal necrolysis (TEN).
-
Diffuse maculopapular rash in toxic epidermal necrolysis (TEN).
-
Toxic epidermal necrolysis (TEN) blister on the index finger.
-
Epidermal sloughing in toxic epidermal necrolysis (TEN).